Author: Michael John Stewart / Editor: Jonathan D Whittaker / Reviewer: Michael John Stewart, Louise Burrows / Codes: / Published: 18/01/2021
Context
Most external eye infections pose little risk to life or vision. Orbital cellulitis is the exception. While antibiotics have reduced the historical mortality rate from 17%, blindness of the affected eye still occurs in 11% of patients1,2. The emergence of antibiotic resistant strains of bacteria has led to a recent increase in this rate even amongst those receiving prompt treatment3,4.
The vast majority of external eye infections are benign, self-limiting conditions. The challenge for the emergency physician is to provide appropriate advice and reassurance for these patients while correctly identifying those with life- or sight-threatening problems.
Learning Bite
Although most external eye infections are relatively benign, orbital cellulitis still carries a significant risk of blindness in the affected eye.
Definition
For convenience, external eye infections can be grouped into four sets:
1. Infections of the lacrimal apparatus
a. Dacryocystitis, involving the draining canaliculi and lacrimal sac
b. Dacryoadenitis, involving the lacrimal gland
2. Infections of the eyelid and associated glands
a. Blepharitis, involving the skin of the lid margin
b. Hordeolum (commonly called a stye), which may be external (pilosebaceous glands on the anterior surface of the eyelid) or internal (infection of the Meibomian glands)
c. Chalazion (Meibomian cyst) is a granulomatous cyst of the meibomian gland.
d. Although not typically infective, chalazia can form as a result of unresolved internal hordeolum
3. Pre-septal (periorbital) cellulitis
Infection of the skin and soft tissues anterior to the fibrous septum
4. Orbital cellulitis
Infection of the soft tissues posterior to the fibrous septum
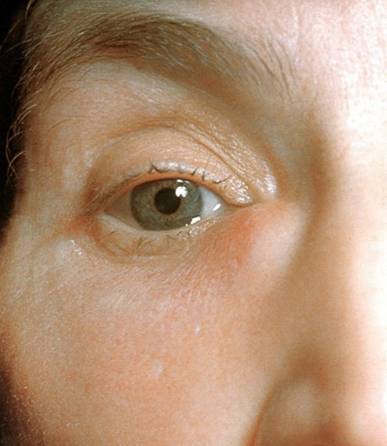
Orbital cellulitis (Reproduced with permission from Wellcome Images)
Basic Science and Pathophysiology
Anatomy of the Lacrimal Glands and Tear Production
The tear film is produced predominantly by the lacrimal glands lying supero-medial to the eye. The basic secretion is water and salts in concentrations similar to plasma, with some additional proteins including lysozyme. This aqueous layer is then covered by a lipid secretion from the meibomian glands lying in the eyelids just posterior to the hair follicles. This secretion limits evaporation of the tear film, and helps to prevent the film leaking from the corners of the eyes.
The tear film drains from the punctum lacrimale found at the medial third of the upper and lower eyelids, travelling via canaliculi to the lacrimal sac adjacent to the eye. The sac drains via the nasolacrimal duct to open in the inferior meatus of the nose.
The lacrimal apparatus
Eyelids and Orbital Soft Tissues
The soft tissues of the orbit are divided by a tough, fibrous septum that arises from the periosteum of the bony structure of the orbit circumferentially, and becomes thickened to form the tarsal plates of the upper and lower eyelids. This divides the soft tissues of the orbit into the pre-septal areas, and the more constrained post-septal space.
Orbital septum(Reproduced with permission from Wellcome Images)
Pathophysiology of External Eye and Lacrimal Infections
Typical organisms depend on the site of infection:
1. Infections of the lacrimal apparatus
Dacryoadenitis is often viral in aetiology, although gram positive cocci (usually staphylococci) are not uncommon.
Dacryocystitis is usually a result of secondary infection, most commonly gram positive cocci 6 and anaerobes, of an obstructed system caused by:
- Tumour
- Trauma
- Congenital malformation
- As a result of local infection
- Mucus plugging in dry eyes
2. Infections of the eyelid and associated glands
When infective, blepharitis and hordeolum are almost exclusively caused by Staphylococci 7. Blepharitis is often a non-infective local dermatitis, and can also be caused by viruses (e.g. Herpes Simplex), mites or lice.
3. Pre-septal cellulitis
The majority of cases are due to bacteria entering after local trauma (e.g. insect bites) of the skin. As such the most common infecting organisms are skin commensals such as staphylococcus aureus and streptococcus pyogenes 8. Less commonly, pre-septal cellulitis may be caused by spread from local infections, including the sinuses. Organisms in these cases are similar to those for orbital cellulitis.
4. Orbital cellulitis
The most common cause (more than 90% of cases) is direct spread from the ethmoid sinuses. Other causes are:
- Direct spread from other structures around the orbit
- Local trauma permitting bacterial entry
- Haematogenous spread from distant site of infection.
Consequently the most common causes of infection are respiratory pathogens such as Streptococci and Haemophilus influenzae type B (the latter less commonly since the introduction of routine HiB immunisation) 8.
Learning Bite
A wide range of gram positive and negative organisms can cause orbital cellulitis. Consideration of the likely underlying cause and route of spread can help to guide antibiotic choice.
History
A more comprehensive account of the clinical assessment of acute eye problems can be found in the Initial Assessment of the Eye Session.
When dealing with a patient with an external eye infection, a full history must be taken including:
- When and where did it start?
- How long has it persisted?
- What symptom(s) is the patient most aware of?
- Is there visual disturbance? this is a worrying sign and should be taken seriously
- Has this occurred before? hordeolum, chalazion, and blepharitis may all recur in the same patient.
- Is there any preceding history of trauma, major or minor, to suggest a route of entry for infection?
- Has there been any recent respiratory tract infection to act as a local source of infection?
Rapidly progressive symptoms are a worrying feature and can be an indicator of more serious disease.
The clinician must resist the temptation to focus solely on the eye. The presence of systemic features can suggest a more serious infection, while diabetes should prompt minor infections to be taken more seriously.
Learning Bite
The presence of visual disturbance or rapidly progressing symptoms should alert the emergency physician to the likelihood of a more significant underlying problem.
Examination
The following points are particularly important when dealing with a patient with an external eye infection;
Features to look for on examination of the face are:
- Evidence of local trauma (including insect bites)
- Swelling overlying the lacrimal sac if so apply gentle pressure and look for the expression of pus at the punctum that indicates dacryocystitis
- Assess the salivary glands Mikulicz syndrome comprises dacryocystitis with dry mouth and swelling of the salivary glands. While the condition itself is benign, it is generally a result of systemic disease, including SLE and lymphoma.
Dacryocystitis (Reproduced with permission from Wellcome Images)
Inspect the eye and surrounding structures for:
- Erythema
- Swelling localised e.g. over the lacrimal gland, periorbital or confined to the eyelid
- Chemosis (conjunctival oedema)
If any or all of these are present, note the location, spread, and anatomical relationships to the eye structures.
Examination of the eye must also include:
- Visual acuity measurement
- Pupillary reaction to light, including relative afferent pupillary defect (RAPD)
- Fundoscopy to assess for papilloedema
- Intra-ocular pressure measurement if available
The presence of any of the following in the context of infection should raise the suspicion of orbital cellulitis
- Proptosis
- RAPD
- Restriction of eye movements or associated diplopia
In addition, be alert to signs of local or systemic spread of infection, including pyrexia, tachycardia, purulent discharge from the nose, or evidence of otitis media.
Learning Bite
While soft tissue infections of the eye are generally minor, they can be a marker for an underlying systemic disease; for example type II diabetes mellitus may present with orbital cellulitis.
Pre-septal cellulitis is a superficial soft tissue infection that should be considered with respect, but is usually amenable to treatment. Orbital cellulitis is a serious, sight-threatening and occasionally life-threatening disease. The two can look similar, especially in the early stages, but there are clues that point to one or the other. The table below summarises the key findings.
|
Pre-septal cellulitis
|
Orbital cellulitis
|
|
|
Local erythema
|
Common
|
Common
|
|
Chemosis
|
Rare
|
Common
|
|
Proptosis
|
Not a feature
|
Common
|
|
Painful eye movements
|
Rare
|
Common
|
|
Restricted eye movements
|
Not a feature
|
Later sign
|
|
Reduced visual acuity
|
Not a feature
|
Late sign
|
|
Systemic features
|
Well
|
Unwell
|
|
Preceding eyelid trauma/infection
|
Common
|
Rare
|
|
Preceding remote infection*
|
Rare
|
Common
|
(*Commonly sinusitis or other upper respiratory tract infection)
If there is a doubt as to the diagnosis, an urgent opinion should be requested from a senior doctor in the emergency department or an ophthalmologist.
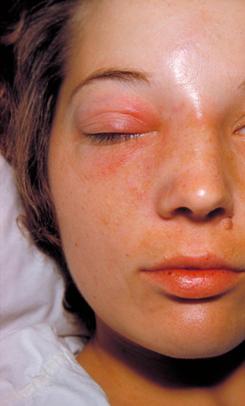
Pre-septal cellulitis (Reproduced with permission from CDC)
Orbital Cellulitis (reproduced with permission from Wellcome Images)
Most external eye infections do not require any specific investigations. As with all infections, a set of baseline observations (including temperature and capillary blood glucose) are useful to identify the systemically unwell. Pre-septal cellulitis, hordeolum, chalazion, blepharitis, and dacryocystitis are all clinical diagnoses.
Orbital cellulitis should be investigated along the lines of other severe infections. Swabs should be taken from any local wounds or discharge from sinuses, and blood should be taken for routine tests and blood cultures.
Further investigation of orbital cellulitis would normally be guided by the ophthalmology team after admission:
- Blind aspiration of the orbit should not be performed. The technique rarely yields diagnostic samples, and carries a significant morbidity.
- If there is any evidence of meningism to suggest spread of infection beyond the orbit, a lumbar puncture should be performed with CSF sent for urgent gram stain.
- HRCT scanning of the orbits can help to confirm the diagnosis, and will indicate spread to deeper structures and guide the need for surgical management.
Learning Bite
With the exception of orbital cellulitis, no investigations other than baseline observations, should be routinely performed in the majority of patients with an external eye infection.
CT scan of orbital cellulitis showing proptosis (Reproduced with permission from Wellcome Images)
Any patient with infection around the eyes should be advised to refrain from wearing contact lenses or eye make-up until it has completely resolved.
Consideration should be given to management of any predisposing condition e.g. sinusitis which may need treatment and occasionally, separate referral and follow-up.
Minor eye infections should not cause a significant change in visual acuity. Patients should be counselled to seek urgent review if this develops.
Dacryoadenitis and Dacryocystitis
Viral Dacryoadenitis (Reproduced with permission from Wellcome Images)
Viral dacryoadenitis, usually occurring with a systemic viral illness (e.g. Mumps, Epstein-Barr virus), is typically self-limiting with treatment aimed at symptomatic relief with analgesia. If bacterial infection is suspected (e.g. isolated swelling without intercurrent viral illness), a course of oral antibiotics is indicated.
Acute dacryocystitis (Reproduced with permission from Wellcome Images)
As dacryocystitis is normally caused by secondary bacterial infection of an obstructed lacrimal system, antibiotic treatment is required. Anaerobic organisms may be present, and therefore an agent providing some anaerobic cover (e.g. co-amoxiclav) is advised.
Occasionally, in non-responding cases, surgical drainage may be required and is important to prevent recurrence. All patients presenting to the ED with dacryocystitis should be referred to an ophthalmologist for follow up.
Learning Bite
Dacryocystitis may require surgical drainage and all patients must be followed up by an ophthalmologist.
Hordeolum
Acute hordeolum
Superficially an acute hordeolum and chalazion will look similar. However, there are a number of differences, largely due to the infective nature of hordeolum as opposed to the granuloma of a chalazion. This table summarises the key differences:
|
Hordeolum
|
Chalazion
|
|
|
Duration
|
Usually less than seven days
|
Can persist indefinitely
|
|
Onset
|
Rapid; can appear overnight
|
Gradual increase in size
|
|
Appearance
|
Red swelling, pus collection may be visible
|
Red/yellow swelling, more rounded
|
|
Discharge from lesion
|
Yes; often noticeable in the morning
|
No
|
|
Tenderness
|
Tender
|
Mild or no tenderness
|
|
Associated problems
|
Can cause local cellulitis or conjunctivitis
|
Usually none
|
An uncomplicated hordeolum will rarely require antibiotic therapy. Application of a warm compress for fifteen minutes at a time, four times a day will encourage the collection to discharge. No review is needed in most cases.
Occasionally complications arise from spread of infection; pre-septal cellulitis should be treated as detailed below, conjunctivitis will require topical antibiotic treatment.
Chalazion
Chalazion (reproduced with permission from Wellcome Images)
Chalazia will often resolve spontaneously, although application of warm compresses four times a day and gentle eyelid massage may speed this up. As they are a granulomatous condition, antibiotics are of no benefit.
Persistent cysts can be referred to an ophthalmologist for elective incision and curettage. This is not an urgent intervention, and can be arranged as an outpatient referral or via the patients GP.
A presumed cyst can be misleading; tumours, including basal cell carcinoma, sebaceous carcinoma, and keratoacanthoma can occur on the eyelid. These can be locally invasive, and sebaceous carcinoma had a 30% five year mortality in one study 9. If in doubt an ophthalmology or dermatology opinion should be sought.
Blepharitis
Blepharitis (reproduced with permission from Wellcome Images)
Advice regarding eye cleaning will resolve many cases of blepharitis. Application of a warm compress, then cleaning with cotton buds dipped in a dilute solution of sodium bicarbonate or mild (baby) shampoo one to three times a day is often effective. If there is evidence of superadded infection, then a course of topical antibiotic ointment (e.g. chloramphenicol) may be required.
It is important to consider precipitating causes such as dry eyes; artificial tears may be of benefit in this situation.
Warn the patient that even once resolved, blepharitis will often recur.
Pre-septal cellulitis
Pre-septal Cellulitis (Reproduced with permission from CDC)
Most patients with pre-septal cellulitis can be managed with oral antibiotics (e.g. co-amoxiclav) on an outpatient basis, with daily review in ED or ophthalmology review clinic, according to local policy 8.
Admission and intravenous antibiotic therapy should be considered:
- If there is doubt as to the diagnosis, especially if orbital cellulitis is possible
- Where there is progression or failure of resolution despite oral therapy
- If there are signs of systemic illness
If a patient is going to be discharged, they should be carefully counselled to seek urgent review if their condition deteriorates.
Learning Bite
Eyelid lesions with atypical appearance or behaviour should be referred for urgent ophthalmic or dermatological review.
Orbital cellulitis
Orbital Cellulitis (Reproduced with permission from Wellcome Images)
When assessing and managing orbital cellulitis, systemic sepsis must be considered, and resuscitation in accordance with standard sepsis guidelines should be initiated10.
Uncomplicated cases of bacterial orbital cellulitis can be managed with IV antibiotics and observation 8,11. Surgical intervention is generally indicated if there is:
- Relative afferent pupillary defect in the affected eye
- Visual loss
- Proptosis
- Lack of progress despite appropriate antibiotic treatment
- Fluid collection seen on CT scan
Learning Bite
If there is any doubt as to whether a patient has pre-septal or orbital cellulitis, a second opinion must be sought from an ophthalmologist or senior ED doctor. Orbital cellulitis is a medical emergency, requiring prompt initiation of IV antibiotics and referral to an ophthalmologist.
The following are some of the common pitfalls that may trap the unwary clinician when dealing with a patient with an external eye infection:
- Mistaking pre-septal cellulitis for orbital cellulitis
- Confusing chalazion with acute hordeolum
- Failure to assess and document visual acuity
- Not ensuring arrangements are made for reviewing significant infections
- Failure to counsel patient regarding cues to seek further review
Key Learning Points
- External eye infections are common, and, although most cases are relatively benign, orbital cellulitis still carries a 1 in 10 risk of blindness in the affected eye. (Level of evidence 4)
- Visual disturbance of rapid progression of symptoms are warning signs or more serious infection. (Level of evidence 5)
- In external eye infections other than orbital cellulitis, no investigations should be routinely performed except a set of baseline observations. (Level of evidence 5)
- Although usually responsive to oral antibiotics, dacryocystitis may require surgical drainage and all patients must be followed up by an ophthalmologist. (Level of evidence 5)
- Eyelid lesions with an atypical appearance are possible malignancies and should be referred for specialist review. (Level of evidence 4)
- Most simple eyelid infections can be treated with simple hygiene measures, and occasionally topical antibiotics. (Level of evidence 5)
- If there is any doubt in differentiating between pre-septal and orbital cellulitis, then the patient should be reviewed by a senior ED physician or an Ophthalmologist. (Level of evidence 5)
- Orbital cellulitis requires in-patient treatment with IV antibiotics. (Level of evidence 4)
- Rutar T, Zwick OM, Cockerham KP, et al. Bilateral blindness from orbital cellulitis caused by community-acquired methicillin-resistant Staphylococcus aureus Am J Ophthalmol. Oct 2005;140(4):740-2
- Jackson K, Baker SR. Clinical implications of orbital cellulitis Laryngoscope. May 1986;96(5):568-74
- Blomquist PH. Methicillin-resistant Staphylococcus aureus infections of the eye and orbit (an American Ophthalmological Society thesis). Trans Am Ophthalmol Soc. 2006;104:322-45
- Boden JH, Ainbinder DJ. Methicillin-resistant ascending facial and orbital cellulitis in an operation Iraqi Freedom troop population. Ophthal Plast Reconstr Surg. Sep-Oct 2007;23(5):397-9
- Hospital Episode Statistics. Inpatient data http://www.hesonline.nhs.uk (accessed 8th December 2009)
- Mills DM, Bodman MG, Meyer DR, et al. The microbiologic spectrum of dacryocystitis: a national study of acute versus chronic infection. Ophthal Plast Reconstr Surg. Jul-Aug 2007;23(4):302-6
- McCulley JP. Blepharoconjunctivitis. Int Ophthalmol Clin. 1984; 24(2):65-77
- Jones DB, Steinkuller PG. Strategies for the initial management of acute preseptal and orbital cellulitis. Trans Am Ophthalmol Soc. 1988;86:94-108
- Kass LG, Hornblass A. Sebaceous carcinmoma of the ocular adnexa
- Surv Ophthalmol 1989; 33:477
- 10. Dellinger RP, Levy MM, Carlet JM, et. al. Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008 Crit Care Med 2008; 36:296-327
- Bergin DJ, Wright JE. Orbital cellulitis. Br J Ophthalmol. Mar 1986;70(3):174-8
- NHS Digital: Hospital Episode Statistics, Admitted Patient Care – England, 2014-15
















12 Comments
comprehensive
Very thorough almost full Ophthalmological disorders covered
Good module
I like the classifications of external eye infection and DD of periorbital and orbital cellulitis
very interesting, with fantastic explanataion
Comprehensive. Very helpful for my portfolio learning!
Great module. many thanks.
Very concise but complete information
thank you
very informative thank you
Wonderfully organized and presented, Thanks a lot
Very useful and concise module, thanks