Author: Jonathan D Whittaker / Editor: Jonathan D Whittaker / Reviewer: Iolo Roberts, Chris Wearmouth / Codes: EC11, EC13, EC2, EC3, EC9, EP6, SLO1, SLO3, SLO5 / Published: 05/08/2022
Context
Sore throat accounted for 1.9% of all visits to emergency departments in the USA in 2006 (1). This figure represents a small percentage of the total disease prevalence as only about 15% of people with an upper respiratory tract infection seek medical care (2).
Most sore throats have an unknown or viral aetiology but group A haemolytic streptococcus (GABHS) is identified as the infecting agent in approximately 5 – 15% of all cases (3). GABHS infection may be complicated by significant sequelae such as rheumatic fever, peritonsillar abscess (quinsy) and post-streptococcal glomerulonephritis.
Even though the vast majority of patients with a sore throat have a benign, self-limiting course, one study found that 64% of primary care patients in the UK are prescribed antibiotics for a sore throat (4).
A recent Cochrane review showed that antibiotics give only modest symptomatic relief and only significantly reduce the risk of serious complications in areas where such complications e.g. rheumatic fever are common. (Spinks A, Glasziou PP, Del Mar CB. Antibiotics for sore throat. Cochrane Database Syst Rev 2013.updated)
Learning Bite
Although the minority of sore throats are caused by bacterial infection, almost 2/3 of patients are managed with a course of antibiotics.
Definition
Patients presenting with a sore throat are commonly diagnosed as having either pharyngitis or tonsillitis. However, it is more accurate to consider these diagnoses as part of a spectrum of a single disease process, tonsillopharyngitis, which encompasses infection or inflammation of the pharynx and/or tonsils.
Rarer, more serious problems such as peritonsillar abscess, epiglottitis and retropharyngeal abscess may also present with the symptom of a sore throat, and must be carefully differentiated from tonsillopharyngitis.
Learning Bite
Patients diagnosed with either tonsillitis or pharyngitis should be considered to have an illness which lies within the spectrum of tonsillopharyngitis.
Group A β haemolytic streptococcus (streptococcus pyogenes) is the infective agent responsible for the most serious complications of tonsillopharyngitis (image, above, reproduced with permissions from CDC).
The M protein GABHS is associated with diseases outside the pharynx, and it is the similarity of some of the serotypes to myocardial sarcolemma antigens that is responsible for the development of rheumatic fever in some patients.
A different process of antigen/antibody complex deposition in glomeruli is responsible for the development of post-streptococcal glomerulonephritis.
Exotoxins
GABHS may also release a variety of exotoxins which are responsible for illnesses such as toxic shock syndrome and necrotising fasciitis. One of these exotoxins, streptolysin O, provokes a reliable immune response which can be measured via the antistreptolysin O titre (ASOT), a standard marker of GABHS infection.
Carriage rates
GABHS may be carried asymptomatically, maximally between the ages of 3 and 15, where carriage rates have been found between 5% and 21%. In adults, the rates are far lower, lying between 2.4% and 3.7% [5].
Complications
Untreated GABHS infection normally lasts between 8-10 days with patients remaining infectious during, and one week after, the illness. Complications of GABHS infection are categorised into suppurative and non-suppurative.
Suppurative complications
Suppurative complications such as otitis media, sinusitis and peritonsillar abscess arise from direct spread of infection into adjacent structures.
Non-suppurative complications
Non-suppurative complications are far rarer with the most common, rheumatic fever, having an annual incidence of less than 10 cases per 100,000 in western Europe and the USA [6].
However, 95% of new cases worldwide occur in the developing world (6) where rheumatic fever remains a significant problem and is responsible for approximately 500,000 deaths annually [7].
Learning bite
Although rheumatic fever is a rare complication of GABHS infection in the western world, it remains a significant problem in the developing world.
History
In taking a history from a patient with a sore throat, the clinician must enquire about the course and duration of illness as well as other associated symptoms such as fever, headache and vomiting. In severe cases, the ability to swallow may be lost and lead to symptoms and signs of dehydration.
Severe pain, neck stiffness or inability to swallow should also prompt the clinician to consider other, more serious, diagnoses such as epiglottitis and retropharyngeal abscess.
Abdominal symptoms such as pain and vomiting are common in children but the presence of gastrointestinal symptoms does not predict the presence of a streptococcal illness [8].
It is important to identify any history suggestive of immunosuppression or compromise e.g. diabetes, HIV or immunosuppressive medications. Patients on disease-modifying anti-rheumatic drug (DMARDs), carbimazole and chemotherapy may develop neutropaenia or agranulocytosis that present with a sore throat. These patients require an urgent Full Blood Count.
The patient must also be asked about previous non-suppurative complications of GABHS infection, as there is an increased risk of both rheumatic fever and post-streptococcal glomerulonephritis with further GABHS infection.
General Examination
An initial ABC assessment may indicate signs of airway obstruction, respiratory difficulty and circulatory collapse. These findings should prompt the junior clinician to seek experienced help immediately.
Signs of upper airway obstruction:
- Snoring
- Gurgling and/or pooling of saliva
- Stridor
- Hoarse voice
- In complete obstruction paradoxical chest movements
It is important to conduct a general examination of the patient as it may reveal;
- Systemic features of infection such as fever and tachycardia
- Heart murmurs found in rheumatic fever
- Neck stiffness which may indicate lymphadenopathy or rarely, retropharyngeal abscess
- Hepatosplenomegaly found in infectious mononucleosis
- Rash which may be viral in origin but also consider;
Rheumatic fever erythema marginatum
Scarlet fever a rough textured macular rash with confluence in the skin folds (Pastias lines) and red cheeks with perioral sparing.
Examination of the face and neck may identify suppurative complications of GABHS infection e.g. otitis media, mastoiditis, sinusitis. Lymphadenopathy in the neck is common in both viral and GABHS infection but the presence of conjunctivitis is more specifically associated with adenoviral infection.
Examination of the mouth and pharynx should be undertaken with care, in particular do not use a tongue depressor if there are any signs of potential airway obstruction as you may worsen the situation.
Learning Bite
Take care when examining the throat as over-vigorous examination or unnecessary painful procedures may worsen or precipitate airway obstruction.
Specific findings may include:
|
Finding
|
Diagnosis
|
|
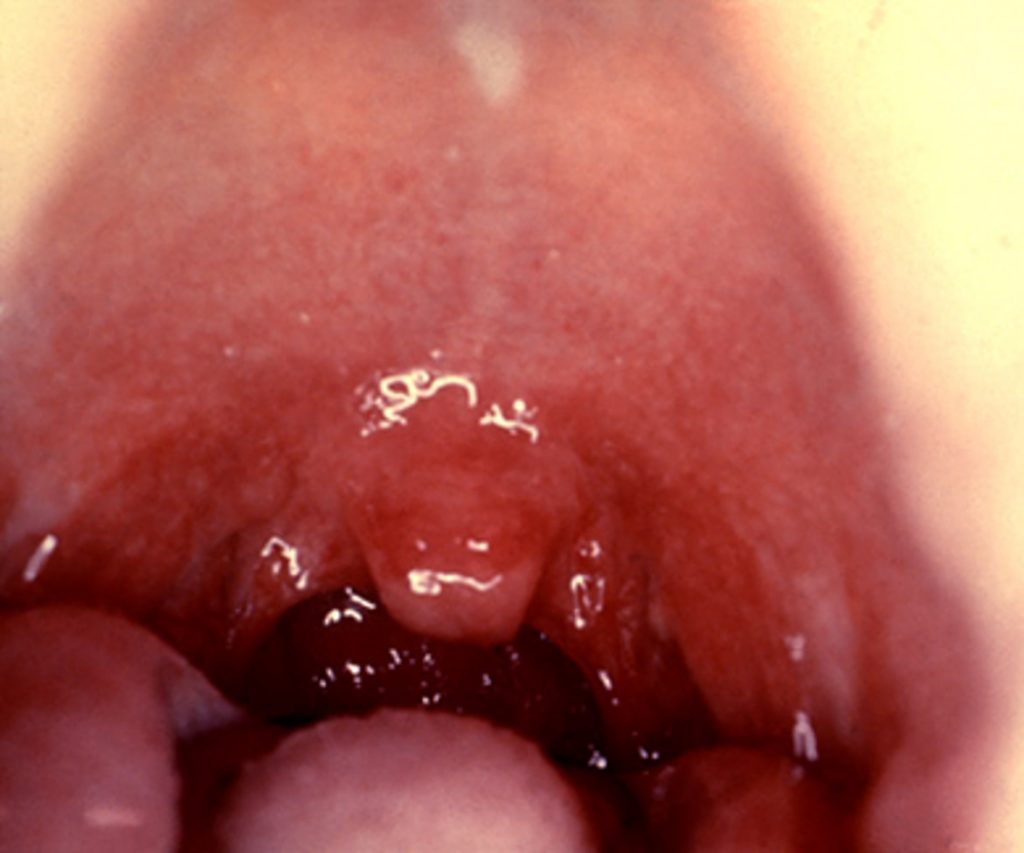
Tonsillopharyngeal or palatal petechiae
|
GABHS infection or infectious mononucleosis
|
|
Unilateral peritonsillar swelling
|
Peritonsillar abscess
|
|
Grey pseudomembrane on the pharynx
|
Diphtheria
|
|
Strawberry tongue
|
Scarlet fever or Kawasakis disease
|
|
Posterior pharyngeal swelling or oedema
|
Retropharyngeal abscess
|
Palatal petechiae in GABHS infection
There are a number of red flag symptoms and signs that should prompt the clinician to consider a more serious cause for a sore throat, including:
- Significant systemic upset
- Severe pain
- Stridor
- Severe neck stiffness
- Inability to swallow / drooling of saliva
- Patient holding a tripod position
A patient with signs of potential or partial airway obstruction such as stridor, inability to swallow and holding a tripod position must be assessed urgently by a senior anaesthetist and otolaryngologist. In this situation the patient must not be moved unnecessarily or have any painful procedures undertaken, such as cannulation or blood gas sampling, until specialist support arrives.
Learning Bite
Patients with impending airway obstruction may present with a sore throat. A patient with stridor, inability to swallow or adopting a tripod position must be managed carefully and with senior anaesthetic and otolaryngology support.
Group A Streptococcal infection is more likely in the winter/spring, and in children aged 5-15.
To differentiate between viral causes, and the potentially more serious GABHS infection, a number of tools have been developed to assess the probability of GABHS infection and therefore the need for antibiotic treatment.
The two recommended by NICE [15] are FeverPAIN and CENTOR.
FeverPAIN Score 0-5 (Each scores 1 point)
⦁ Fever over 38°C.
⦁ Purulence (pharyngeal/tonsillar exudate)
⦁ Attend rapidly (3 days or less)
⦁ Severely Inflamed tonsils
⦁ No cough or coryza
CENTOR Score 0-4 (Each scores 1 point)
⦁ Tonsillar exudate
⦁ Tender anterior cervical lymphadenopathy or lymphadenitis
⦁ History of fever (over 38°C)
⦁ Absence of cough
A modified version of CENTOR adds in age to increase accuracy, but is not currently included in NICE guidance [10].
Scores and subsequent likelihood of isolating Streptococcus [15].
| FeverPAIN | CENTOR | ||
|---|---|---|---|
| 0 – 1 | 13 – 18% | 0 | 3% |
| 2 – 3 | 34 – 40% | 1 | 7% |
| 4 – 5 | 62 – 65% | 2 | 15% |
| 3 | 32% | ||
| 4 | 56% | ||
Learning bite
A sore throat score is useful in predicting the likelihood of GABHS infection and can reduce unnecessary antibiotic prescriptions by 50%.
Note that these scores are not applicable to other causes of sore throat other than tonsillopharyngitis.
There are a number of strategies that can be employed in the investigation of patients with a sore throat:
Rapid streptococcal antigen testing
In the USA, and other countries without universal primary care backup, rapid streptococcal antigen testing has been widely utilised in the ED. The test is claimed to be 95% sensitive and specific but, in some studies, sensitivity has varied between 55% and 90% and has also been found to vary considerably depending on the operator performing the test [12].
In one study carried out in UK ED setting, rapid streptococcal antigen testing was found to have a sensitivity of 66% but 99% specificity [13]. Although included in NICE guidance, not all UK EDs have access to rapid streptococcal antigen testing.
Antistreptolysin O titre (ASOT)
A rising antistreptolysin O titre (ASOT) provides the gold standard criteria for immunologically significant GABHS infection. However, it is impractical and unnecessary in the vast majority of cases of sore throat.
Throat swab
Throat swabs, although widely used, are reliant on correct technique and interpretation is complicated by asymptomatic carriers of GABHS.
Covid-19 swab
It is recognised that sore throat can be a symptom of Covid-19. By itself it is not necessitate a PCR test, however clinicians should consider if there are other symptoms such as fever, new continuous cough or loss/change to sense or taste or smell [24].
Other investigations
Other investigations which may be useful in patients with a sore throat include:
- Routine bloods should be taken if the patient is being cannulated for another reason e.g. unable to swallow. These may show signs of dehydration
- FBC will likely show leucocytosis. A raised WBC count with lymphocytosis and atypical lymphocytes is suggestive of infectious mononucleosis
- Heterophile antibody tests for infectious mononucleosis e.g. Monospot and Paul Bunnell tests
- Deranged liver function tests are present in 90% of patients with Infectious Mononucleosis
- Chest x-ray if respiratory infection is suspected
- Fibreoptic Nasal Endoscopy (FNE) can be performed by ENT specialists in ED to visualise the pharynx and glottis. It is particularly of use in patients presenting with stridor
- Lateral soft tissue neck x-ray for retropharyngeal abscess and epiglottitis.
An epiglottic width (widest anteroposterior diameter of the epiglottis) of >7 mm was found to have a sensitivity and specificity of 100% for the diagnosis of epiglottitis in one study [14] (see image below).
Tonsillopharyngitis
The current recommended strategy for the management of uncomplicated tonsillopharyngitis in the UK relies on a pragmatic expectant policy i.e. no initial antibiotics are given and the patient is advised to return to their GP if their symptoms are not settling after a few days [15].
Expectant management
The strategy of expectant management is based on a Cochrane review of antibiotics for sore throat [16]. This found that a course of antibiotics has minimal effect on the course of the illness, shortening it by approximately 16 hours.
Another study found that an antibiotic prescription increases the chance of a patient with a sore throat returning in the future for antibiotics [17]. Despite this evidence, antibiotic prescribing rates remain high. Patient expectation is often quoted as the main reason for this but, in a study conducted in 10 EDs in the USA, patient satisfaction rates were not altered by the decision to prescribe antibiotics for upper respiratory tract infections [18].
Learning bite
Treating an uncomplicated sore throat with antibiotics has little effect on the clinical course of the illness and may encourage patients to return in the future when a similar problem arises. It also increases risk of anti-microbial resistance or side effects.
Antibiotic Prescription
NICE currently advise to consider antibiotic prescription if the FeverPAIN score is 4 or 5, or CENTOR score is 3 or 4, and a rapid streptococcal antigen test is pending or not available. If the FeverPAIN is 2 or 3 then you should consider a delayed antibiotic prescription.
The threshold is lower if the patient is at risk of rheumatic fever or are vulnerable. Antibiotics should not be withheld if the person has very severe symptoms and there is concern about their clinical condition.
Learning Bite
During Covid-19, RCPCH have recommended only examining children’s’ throats if necessary. If not, they recommend assuming a score 2 in lieu of examination [23].
Antibiotic choice
Phenoxymethylpenicillin QDS for 10 days is the first line choice antibiotic. If the patient is penicillin allergic then recommendation is clarithromycin, or erythromycin if they are also pregnant.
Phenoxymethylpenicillin is normally prescribed as a four times daily regime although, in a meta-analysis, similar cure rates were found for twice daily dosing [19] with consequent better compliance rates.
Amoxicillin and other Ampicillin antibiotics should be avoided in sore throat due to the possibility of causing maculopapular exanthems in patients with infectious mononucleosis.
Other treatment
Simple analgesia including paracetamol, non-steroidal anti-inflammatories and topical local anaesthetic agents (e.g. Benzydramine spray/mouthwash) are effective in patients with a sore throat and may have a greater positive effect than antibiotics alone.
Steroids such as Dexamethasone are frequently used in hospital if the patient is unable to swallow due to severe pain or has stridor.
Other diagnoses
Learning bite
Regardless of the underlying cause, always assess the patient for signs of airway obstruction or dehydration that may require admission.
Common cold
The majority of sore throats are viral in origin. Suggested by rhinorrhoea, coryza, and cough. Can be managed with simple analgesia and rest.
Scarlet fever
Scarlet fever is a GABHS exotoxin-mediated illness which occurs far more commonly in children. Other than standard antibiotic treatment for GABHS, consideration must also be made of hydration status and intravenous fluid rehydration may be required. It is a notifiable disease in England and Wales.

Peri-tonsillar Abscess (Quinsy)
Uncomplicated peritonsillar abscess may be managed in the ED although it is common practice for patients to be referred to an ear, nose and throat (ENT) specialist due to a lack of familiarity with treatment techniques.
Both needle aspiration and incision and drainage techniques may be employed, and have been found to be equally effective [21]. The clinician must be aware of the potential complications of both the problem e.g. Lemierre’s syndrome (extension of infection involving the jugular vein) and its management e.g. accidental puncture of the carotid artery.
Learning bite
Peritonsillar abscess can be treated equally effectively by either needle aspiration or incision and drainage, although the operator must be familiar with both the technique and the potential serious complications.
Patients should receive a broader antibiotic choice than standard pharyngotonsillitis as organisms other than Group A Streptococcus are also likely to be causative (follow local Microbiology guidance).
Infective Mononucleosis
Caused by the Ebstein Barr virus. Suggested by prolonged symptoms, fatigue, generalised lymphadenopathy and hepatosplenomegaly. More common teenagers and young adults. Advise patients that symptoms can take weeks to months to resolve. Patients should avoid kissing and sharing towels or kitchen utensils. They should avoid heavy lifting or contact sports for 1 month due to the risk of splenic rupture. Advise them to return to ED in the event of sudden onset abdominal pain [25].
Learning bite
HIV may present as a sore throat with myalgia, arthralgia, lymphadenopathy and lethargy during seroconversion. Patients being investigated for suspected Infectious Mononucleosis should be considered for HIV testing as well.
Epiglottitis/Supraglottitis
Since the advent of Hib vaccination, epiglottitis is now more commonly an infection affecting adults. The main complication of airway obstruction may be predicted by the presence of specific clinical features [22]:
- Stridor
- Muffled voice
- Rapid clinical course
- History of diabetes
Any patient presenting with these features should be urgently reviewed by anaesthetics and ENT.
A review of 106 patients with epiglottitis found that routine intubation was unnecessary as over 90% of patients recovered with a conservative watchful approach [23].
The main focus of treatment centres on observation for airway obstruction and administration of antibiotics – a third-generation cephalosporin and metronidazole are recommended to cover the spectrum of organisms responsible. Adrenaline nebulisers and Dexamethasone is commonly given to reduce swelling.
Learning bite
Since the advent of Hib immunisation, epiglottitis has become more common in adults and, in the absence of high risk features, can normally be managed with antibiotics and careful observation.
Retropharyngeal Abscess
Although very uncommon, a combination of sore throat, fever, neck stiffness and stridor should alert the clinician to consider this diagnosis. Swelling or oedema of the posterior pharynx should prompt a consideration of advanced airway care and an urgent ENT opinion. Mortality rates are high when complications such as airway obstruction and mediastinitis arise.
- Sore throat is a common presentation to both the ED and primary care and is managed with an over-reliance on antibiotic prescription. (level of evidence 4)
- Non-suppurative complications of GABHS infection are extremely rare in the Western world, although in the developing world, rheumatic fever remains a very significant problem. (level of evidence 5)
- The presence of severe throat pain, stridor, significant systemic upset, neck stiffness, inability to swallow saliva and the patient holding a tripod position are all signs of a more serious cause for a sore throat. (level of evidence 5)
- Clinical features of partial or potential airway obstruction (stridor, altered voice, inability to swallow saliva, tripod position) must be managed by gentle handling of the patient and urgent senior ENT and anaesthetic assessment. (level of evidence 5)
- NICE guidance includes use of both the CENTOR and FeverPAIN scores to assess the likelihood of Group A Streptococcal infection and can reduce unnecessary antibiotic prescription by 50%.
- The treatment of uncomplicated sore throat with antibiotics has little effect on the course of the illness and the use of an expectant or delayed antibiotic policy does not increase the incidence of complications. (level of evidence 1a)
- Simple non-antibiotic treatments such as NSAIDs and paracetamol are effective and may have a larger treatment effect than antibiotics alone. (level of evidence 2a)
- In the absence of features associated with a high risk of airway obstruction, epiglottitis can normally be managed without routine intubation, using a strategy of intravenous antibiotics and close observation. (level of evidence 4)
- Pitts SR, Niska RW, Xu J, Burt CW. National Hospital Ambulatory Medical Care Survey: 2006 emergency department summary. Natl Health Stat Report. 2008 Aug 6;(7):1-38.
- McIsaac WJ, Goel V, To T, Low DE. The validity of a sore throat score in family practice. CMAJ. 2000 Oct 3;163(7):811-5.
- Cooper RJ, Hoffman JR, Bartlett JG, et al., Principles of appropriate antibiotic use for acute pharyngitis in adults: background. Ann Intern Med. 2001 Mar 20;134(6):509-17.
- Petersen I, Hayward AC; SACAR Surveillance Subgroup. Antibacterial prescribing in primary care. J Antimicrob Chemother. 2007 Aug;60 Suppl 1:i43-47.
- Gunnarsson RK, Holm SE, Söderström M. The prevalence of potential pathogenic bacteria in nasopharyngeal samples from healthy children and adults. Scand J Prim Health Care. 1998 Mar;16(1):13-7.
- Tibazarwa KB, Volmink JA, Mayosi BM. Incidence of acute rheumatic fever in the world: a systematic review of population-based studies. Heart. 2008 Dec;94(12):1534-40.
- Carapetis JR, Steer AC, Mulholland EK, Weber M. The global burden of group A streptococcal diseases. Lancet Infect Dis. 2005 Nov;5(11):685-94.
- Kreher NE, Hickner JM, Barry HC, Messimer SR. Do gastrointestinal symptoms accompanying sore throat predict streptococcal pharyngitis? An UPRNet study. Upper Peninsula Research Network. J Fam Pract. 1998 Feb;46(2):159-64.
- Centor RM, Witherspoon JM, Dalton HP, et al., The diagnosis of strep throat in adults in the emergency room. Med Decis Making. 1981;1(3):239-46.
- McIsaac WJ, White D, Tannenbaum D, Low DE. A clinical score to reduce unnecessary antibiotic use in patients with sore throat. CMAJ. 1998 Jan 13;158(1):75-83.
- Rosenberg P, McIsaac W, Macintosh D, Kroll M. Diagnosing streptococcal pharyngitis in the emergency department: Is a sore throat score approach better than rapid streptococcal antigen testing? CJEM. 2002 May;4(3):178-84.
- Fox JW, Cohen DM, Marcon MJ, Cotton WH, Bonsu BK. Performance of rapid streptococcal antigen testing varies by personnel. J Clin Microbiol. 2006 Nov;44(11):3918-22.
- Van Limbergen J, Kalima P, Taheri S, Beattie TF. Streptococcus A in paediatric accident and emergency: are rapid streptococcal tests and clinical examination of any help? Emerg Med J. 2006 Jan;23(1):32-4.
- Yong MG, Choo MJ, Yum CS, Cho SB, et al., Radiologic laryngeal parameters in acute supraglottitis in Korean adults. Yonsei Med J. 2001 Aug;42(4):367-70.
- National Institute for Health and Care Excellence. Sore throat – acute. (Topic review). NICE CKS. Last revised in 2021.
- Del Mar CB, Glasziou PP, Spinks AB. Antibiotics for sore throat. Cochrane Database Syst Rev. 2006 Oct 18;(4):CD000023. doi: 10.1002/14651858.CD000023.pub3. Update in: Cochrane Database Syst Rev. 2013;11:CD000023.
- Little P, Gould C, Williamson I, et al., Reattendance and complications in a randomised trial of prescribing strategies for sore throat: the medicalising effect of prescribing antibiotics. BMJ. 1997 Aug 9;315(7104):350-2.
- Lan AJ, Colford JM, Colford JM Jr. The impact of dosing frequency on the efficacy of 10-day penicillin or amoxicillin therapy for streptococcal tonsillopharyngitis: A meta-analysis. Pediatrics. 2000 Feb;105(2):E19.
- Ong S, Nakase J, Moran GJ, Karras DJ, et al., Antibiotic use for emergency department patients with upper respiratory infections: prescribing practices, patient expectations, and patient satisfaction. Ann Emerg Med. 2007 Sep;50(3):213-20.
- Thomas M, Del Mar C, Glasziou P. How effective are treatments other than antibiotics for acute sore throat? Br J Gen Pract. 2000 Oct;50(459):817-20.
- Broomfield, S. and Saunders, F. Acute management of peritonsillar abscess (quinsy). BestBets. 2005.
- Katori H, Tsukuda M. Acute epiglottitis: analysis of factors associated with airway intervention. J Laryngol Otol. 2005 Dec;119(12):967-72.
- Royal College of Paediatrics and Child Health. COVID-19 – guidance for management of children admitted to hospital and for treatment of non-hospitalised children at risk of severe disease. RCPCH. Last modified in 2022.
- NHS. Coronavirus (COVID-19) symptoms in adults.
- National Institute for Health and Care Excellence. Glandular fever (infectious mononucleosis). (Topic Review). NICE CKS. Last revised in 2021.
- A right sided peritonsilar abscess. James Heilman via Wikimedia. 2011.







25 Comments
common presentation in ED – refresh my knowledge.
A good learning module for a common presentation.
very informative
good concise module
Very informative and relevant. Thank you
Helpful summary
Great simple refreshment about one of the most common presentation
Super helpful module for a common presentation to the paeds ED
nice and simple module, thank u
v good module for refresh my knowledge
fantastic concise module
Nice summary, educative
comprehensive article
Thanking you
Very helpful thank you!
Sore throat is not that simple
good refresher
Good review. Interesting read
good review.
Thanks
thanks
Easy to read
Nice Summary, especially relevant with the current wave of streptococcal infections
Nice fruitful topic
Comprehensive account on throat pain