Author: Henry R Guly / Editor: Jason M Kendall, Phil Delbridge / Reviewer: Jennifer Lockwood / Codes: SLO4, TC2, TP7 / Published: 05/04/2021
Foot injuries are common and because they affect mobility, they can have a significant affects on a patients life and so are important. Unfortunately there is very little evidence for the treatment of these conditions. There are no current relevant Cochrane reviews, NICE nor SIGN guidelines. In a standard orthopaedic textbook of 781 pages, only 11 are devoted to foot fractures [1].
Assessing an X-ray
One system for assessing x-rays is AABCS:
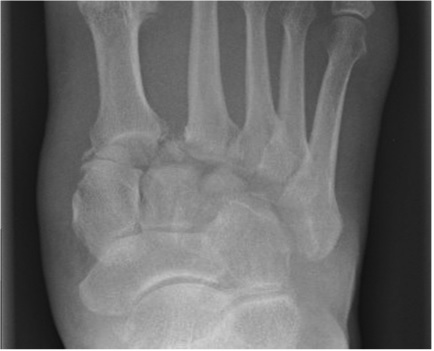
The image displays a normal x-ray (click on the x-ray to enlarge).
A – Adequacy
- Check it is the correct patient and the correct date
- Check that the correct side has been x-rayed, the correct views have been taken and that all the areas of interest are included
A – Alignment
- Is the alignment of the joints correct or is there any dislocation?
- The area where injuries are commonly missed is the tarso-metatarsal joint
B – Bones
- Trace the outline of every bone to ensure no cortical break
- Look at the medulla for trabecular pattern
C- Cartilages
- Look at joint spaces
- Overlapping of bones may indicate a dislocation
S – Soft tissues
Look for:
- Swelling
- Air in tissues, soft tissue calcification, etc.
Visualising Injuries
Injuries of the talus may be seen on ankle x-rays. The lateral x-ray of the ankle and lateral x-ray of the foot are very similar. An AP x-ray of the ankle is shown (Fig 1) and is useful for visualising the talus.
In suspected calcaneal injuries, calcaneal views should be requested (Fig 2). If ankle x-rays are requested, it is not necessary to carry out a specific lateral of the calcaneum as this is just a coned ankle x-ray. However fractures may not always be easily seen on the lateral x-ray so an axial view of the calcaneum is taken.
When looking at the lateral x-ray of the ankle, it is important to look at Bohler’s angle (Fig 3). This should be about 140°. If Bohler’s angle is flattened, this suggests a fracture.
If the mechanism of injury (e.g. a road crash) suggests that there may be other injuries, it is important to complete a full assessment to exclude other injuries. Otherwise, the assessment of a foot injury is the same as the assessment of any other trauma:
History
The mechanism of injury is of vital importance and may give valuable clues towards the diagnosis of injuries to the feet and other associated injuries.
Examples are:
- An inversion injury of the ankle may cause an ankle injury but may also cause a fracture at the base of the 5th MT
- Dropping a weight onto the foot may cause a fracture but is unlikely to cause a dislocation whereas a stubbed toe may cause either a fracture or a dislocation
- With major forces, one should expect serious injuries and some of these may be subtle on x-ray
- The past history may be significant and, in particular, diabetic neuropathy may predispose to a neuropathic arthropathy
Examination
Examination will consist of:
- Look – for deformity, bruising, swelling scars etc.
- Feel – for deformity, point of maximum tenderness
- Move – examine for movement at all the joints – subtalar, midtarsal, toes
- Function – can the patient walk? Examine their gait
- Test for neurovascular function
- Examine the ankle
Learning Bite
The history and mechanism of injury will give valuable clues as to the diagnosis.
X-ray
As noted above, inversion of the ankle may be associated with a foot injury. The Ottawa foot rules [2] (see Figure 1) give evidence-based advice on whom to X-ray. These state that in ankle injuries, foot X-rays are only required if:
There is pain in the midfoot zone and there is either:
1. Bone tenderness at C (the base of the 5th metatarsal) or
2. Bone tenderness at D (the navicular) or
3. Inability to weight-bear (4 consecutive steps) both immediately and in the ED.
Figure 1. Ottawa Ankle Rules

A standard foot series of X-rays consist of an AP, an oblique and a lateral of the foot. However for forefoot injuries, an AP and oblique are usually adequate as on a lateral X-ray of the foot, the metatarsals and the toes overlap and this obscures details. However, occasionally the lateral X-ray may be required to demonstrate any displacement of a fractured metatarsal (especially the 1st).
Suspected talar injuries will require ankle X-rays in addition to foot X-rays
The lateral X-ray is most useful for looking at the hind foot and mid foot and these areas are also well shown on a lateral ankle x-ray so if an ankle X-ray series has been obtained, a lateral foot x-ray will rarely be required
Fractures (and other abnormalities) always show best if the X-ray is centred over the abnormality so, for a toe injury, request X-rays of the toes rather than a foot X-ray.
Calcaneal fractures may not be easy to see on ankle or foot X-rays so if a fracture is suspected, request calcaneal views (a lateral view of the calcaneum or ankle and an axial view of the calcaneum).
Even if you forget to request specific views, if you state the injury you suspect or want to exclude, the radiographer should do the X-rays that you need.
Computed tomography (CT)
CT will often be needed to assess the extent of calcaneal and talar fractures and also mid-tarsal and tarso-metatarsal injuries. CT may also be useful if the diagnosis is not obvious.
Learning Bite
When requesting X-rays, do not write: -Fracture X-ray foot but specify what injury you are expecting and the radiographer should do the views that are most likely to show that injury
Fractured calcaneum
As discussed above, fractures may not be obvious on the lateral X-ray and it is important to obtain an axial view.
On the lateral X-ray, look at Bohler’s angle (Figure 2) which should be approximately 140o. Flattening of this angle suggests a fracture.

Figure 2: Bohler’s angle
Fractures of the calcaneum are the commonest tarsal fractures and usually classified into:
- Extra-articular not involving the subtalar joint
- Intra-articular fractures involving the subtalar joint
Extra-articular fractures
Types:
They include fractures of:
- The medial tubercle (figure 3a),
- The anterior process (figure 3b),
- The tuberosity (figure 3c),
- The sustenaculum tali (figure 3d)
- The body of the calcaneum posterior to the subtalar joint (figure 3e).
Figure 3: Extra-articular fractures of the calcaneum
Figure 3c and Figure 3d
Figure 3e
Management
Treatment in the ED includes:
Treatment in the emergency department (ED) should follow local protocols, if available. If no protocol exists, treatment should be as follows:
- Analgesia, if required
- If there is any doubt about whether the fracture involves the subtalar joint, a CT may be requested
- If it is a displaced fracture, refer for an orthopaedic opinion
Undisplaced extra-articular fractures can be treated with:
- Support bandage (e.g. wool and crepe) or below knee plaster of Paris (POP). It would be expected that patients would regain movement faster without plaster of Paris but there is no evidence for this [2]
- Crutches
- Advice on elevation
- Referral to fracture clinic for follow-up
Prognosis:
These fractures are relatively minor and have a good prognosis
Intra-articular fractures
Intra-articular calcaneal fractures are usually caused by a fall from a height onto the heel. In older patients with osteoporosis, the height may be as little as half a metre. Extra-articular fractures of the body and the medial tubercle are also caused by the same mechanism, though with lesser degrees of force. As patients usually fall onto both heels, bilateral fractures are common.
The same mechanism of injury may also cause a fracture of the lumbar spine and so all patients with calcaneal fractures must have the spine examined. If there is any suspicion of back injury (or if a back injury cannot be ruled out because of distracting pain) the lumbar and thoracic spine must be x-rayed.
Figure 4: Intra-articular fracture of the calcaneum
Figure 4 shows an intra-articular fracture of the calcaneum; the bone texture is abnormal and there are lucencies suggestive of a fracture but there are no obvious breaks in the cortex. Bohlers angle is grossly flattened.
Management:
There are several patterns of intra-articular fractures but the exact patterns need not be known by emergency physicians as all these injuries will be referred to orthopaedic surgeons for further management. They will usually be admitted and investigated further by CT.
There are a variety of treatment options including reconstructive surgery. There is usually severe disruption of the subtalar joint and stiffness and arthritis of this joint is very common.
Prognosis:
There is usually severe disruption of the subtalar joint and stiffness and arthritis of this joint requiring further surgery is very common.
Learning Bite
- If you suspect a fractured calcaneum, ask for specific calcaneal views.
- When looking at a lateral ankle or foot X-ray, always evaluate Bohlers angle
Fractured talus
Fractures of the body of the talus are relatively uncommon injuries and are normally caused by major forces. The common site of a fracture is across the waist and this is caused by forced hyper-dorsiflexion of the ankle. The commonest cause for this is a road crash in which the car-drivers foot is forced backwards in a head-on collision. Injuries can also occur in a fall from a height.
Fractures of the neck of the talus are classified as:
Type I: undisplaced (see Figure 5)
Type II: displaced (however little) and associated with subluxation or dislocation of the subtalar joint (see figure 6)
Type III: displaced with dislocation of the talus from the ankle joint
Undisplaced fractures are easily missed and displaced fractures may be thought to be undisplaced and so CT is valuable in the assessment of talar injuries. As they are high velocity injuries, they may be associated with life-threatening injuries of the head and trunk and may be overlooked.
Dislocation of the talus can occur with or without an associated fracture.
Figure 5. Undisplaced fracture of the waist of the talus (type 1)
Figure 6. Displaced fracture of the talus (type II)
Management:
Truly undisplaced fractures can be treated in a below knee POP.
All others need to be referred to an orthopaedic surgeon as an anatomical reduction is needed and this usually requires ORIF. If the skin is tight over the fracture, this is urgent.
Prognosis:
The major complication of these injuries is avascular necrosis of the proximal part of the bone.
Fractured navicular
Minor avulsion fractures are common, often in association with a sprain of the ankle, and usually require no specific treatment.

Figure 7. Fracture navicular
Isolated fractures of the navicular are uncommon. If they are undisplaced, they will normally be treated conservatively; displaced fractures will need an orthopaedic opinion for consideration of ORIF.
Fractures of the navicular may occur in association with dislocations of the mid-foot. Any significant injury in this area requires a lateral X-ray of the foot in addition to normal foot X-rays. If there is suspicion of a dislocation, CT evaluation is required.
Fractured cuboid
Minor avulsion fractures are common and usually require no specific treatment.
Most fractures are undisplaced and will be treated conservatively. Displaced fractures may be part of a more complex foot injury and will need an orthopaedic review.
Subtalar dislocation
The subtalar joint is the joint between the talus and the calcaneum. If this joint dislocates, the forefoot stays attached to the calcaneum and so the talo-navicular joint also dislocates (see figure 8). Subtalar dislocation occurs in excessive inversion or eversion and can occur medially or laterally. It may be associated with a fracture of the lateral malleolus.
Figure 8. Lateral subtalar dislocation (and fracture of the lateral malleolus)
Management
Ideally the ankle and foot should have an x-ray to confirm the diagnosis. However if it is thought that there is a risk of neurovascular impairment, or if the skin is stretched and there is concern that tightness of the skin may risk skin necrosis, it is common practice to try to significantly reduce displaced ankle and foot injuries before x-ray.
If a displaced fracture is reduced before x-ray, the fracture is still visible and so a diagnosis is still possible. However, if a dislocation is reduced beforehand, the subsequent x-ray may be normal and it may be difficult to establish the true diagnosis.
These injuries should be reduced under sedation, or general anaesthesia, and immobilised in a below knee POP. They should be followed up by an orthopaedic surgeon.
Midtarsal dislocation
In a midtarsal dislocation, the cuboid and navicular dislocate from the talus and calcaneum. The joint may dislocate medially (with an adduction force) or laterally (with an abduction force)
These dislocations may be associated with fractures of the tarsal bones (particularly the navicular) or with smaller avulsion fractures.
In major foot injuries always obtain a lateral X-ray of the foot in addition to the usual AP and oblique views. Similarly if standard X-rays show a fracture of the navicular, obtain a lateral X-ray of the foot.
If there is a significant mechanism of injury and the patient clinically has a fracture with much swelling but the X-rays appear normal or relatively normal, consider doing a CT.
Tarso-metatarsal dislocation (Lisfranc injury)
The tarso-metatarsal joint is also known as the Lisfranc joint and so dislocations at this site are also known as Lisfranc injuries.
These are commonly missed but the clue to their diagnosis is abnormalities in the alignment of the metatarsals with the tarsal bones. Figure 9 shows how the medial border of the 2nd MT normally align with the medial border of the intermediate cuneiform on the AP view and the medial border of the 4th MT should align with the medial border of the cuboid on the oblique view.
Figure 10 shows a severe tarso-metatarsal dislocation with severe misalignment and at least three bony fragments. Fig 11 shows a less obvious tarso-metatarsal dislocation with a small step between the base of the 2nd metatarsal and the intermediate cuneiform.
Figure 9: Normal alignment between tarsus and metatarsals
Figure 10: Severe tarso-metatarsal dislocation
Figure 11: Subtle Lisfranc injury
These injuries need orthopaedic referral. Most will be investigated with a CT and most will be internally fixed.
Not all injuries at this joint are obvious on initial x-rays (click on the x-ray to enlarge). If it is suspected clinically but x-rays are normal, the patient should be kept under review and consideration given for a CT.
Fractures of the 5th metatarsal
Fractures of the 5th metatarsal base in association with an inversion injury of the ankle are avulsion fractures occurring at the insertion of the tendon of peroneus brevis.
They are normally treated symptomatically with either a supportive bandage or plaster, with or without crutches (depending on the patients mobility). Only one study (of low quality) has adequately compared plaster and supportive bandaging. This suggests that there is no difference in pain or time to bony union but that support bandaging significantly shortens the time to full activity and so is recommended. [3]
Most fractures heal quickly but occasionally go to non-union. This only needs treatment if it is symptomatic.
Differentiating Types of 5th Metatarsal Fractures
Fractures at the base of the 5th MT are normally transverse or oblique and in children must be differentiated from the apophysis, which is longitudinal (Fig 1) or even fragmented (Fig 2).
These fractures must also be differentiated from those that occur at the base of the shaft of the 5th MT, commonly referred to as Jones fractures (Fig 3). Though they can occur as a result of trauma, Jones fractures are usually stress fractures. Due to significant incidence of non-union, they are normally managed in plaster and should be referred for orthopaedic follow up.
Other fractures of the shaft of the MT (Fig 4) are treated symptomatically.
Fractures of other metatarsals
Fractures of a single MT, 2nd, 3rd or 4th, (Fig 1) are usually well splinted by the other, intact, MTs and require symptomatic treatment only.
However, fractures of the 1st MT (Fig 2) may displace and therefore sometimes require internal fixation. The presence of multiple MT fractures (Fig 3) allows each fracture to displace. These patients normally require orthopaedic admission for elevation, treatment of soft tissue swelling and to consider internal fixation.
Fractures at the bases of the MTs (except for 5th) may be associated with injuries of the tarso-MT joint.
Crush Injuries of the Foot
A crushed foot may occur if it is run over by a vehicle or if a heavy weight falls on it. The foot will be swollen, bruised and painful. An x-ray may or may not show a fracture and if a fracture occurs, it will usually be to one or more of the smaller MTs.
While any fracture must be treated appropriately, it is important to recognise that the injury is more than just a fracture as there is a major soft tissue injury as well and even if the x-ray is normal, the injury cannot be ignored.
Occasionally there may be an occult fracture (requiring further x-rays or CT) but even if there is not, the soft tissue injury needs treatment to avoid morbidity.
Treatment
Crush injuries require elevation and ice to reduce the swelling. Later they may need physiotherapy.
Patients may be able to elevate their feet at home (they will need crutches) but often need admission and will definitely need referral if there is any possibility of a compartment syndrome.
Toe injuries
Fractures
Most toe fractures will be caused either by dropping a weight on the foot, or by stubbing the toe.
Undisplaced fracture
This x-ray shows an undisplaced fracture. It requires no specific treatment but will usually be treated with neighbour strapping for a few weeks and advice on analgesia and footwear. Most patients seem more comfortable in sandals but some prefer wearing walking boots, or similar, as they are less likely to knock their toe.
Click on the x-ray to enlarge.
Displaced fractures
Significantly displaced fractures require manipulation followed by neighbour strapping.
Click on the x-ray to enlarge.
Fracture proximal phalanx big toe
Displaced fractures of the big toe are obviously more serious than injuries of the other toes and may need internal fixation.
Click on the x-ray to enlarge.
Dislocation
It has been argued that x-rays of clinically undisplaced injuries of the toe are unnecessary as they do not alter treatment. This is only true provided the toe is examined carefully since it is important not to miss a dislocation of the toe that would need reduction. Dislocations can be reduced under local anaesthesia. A post-reduction X-ray should be obtained.
Subungal haematoma

A subungal haematoma is usually caused by a blow to the toe which may, or may not, also cause a fracture. The pressure from it often causes pain and this can be significantly relieved by trephining the nail to allow the release of blood. However there is no evidence to say that this treatment is better than no treatment [4].
It is sometimes argued that patients with an underlying fracture should be given antibiotics as the act of trephining converts a closed fracture to an open one. However antibiotics do not seem to be necessary [5].
Wounds
Tendon and nerve injuries should be examined for any laceration around the foot and the ankle. This patient has divided their extensor hallucis longus tendon.
Puncture wounds
Puncture wounds of the foot are common. A frequent presentation is the patient who treads on a nail sticking up through a plank of wood. This penetrates the shoe and goes into the sole of the foot. There appears to be a significant risk of infection, particularly as the depths of the wound cannot be fully cleaned.
Osteomyelitis is not unknown if the nail penetrates into bone. The wound should be cleaned as much as possible and dressed. If the hole is large, it should be irrigated. Tetanus prophylaxis should be provided. There are many opinions as to whether antibiotics should be used to try to prevent infection but no evidence either for or against this [6].
Foreign bodies
People who walk in bare feet may tread on a sharp object such as a needle or broken glass and present with a foreign body (FB) on the sole of the foot.
If there is any suspicion of a foreign body, an x-ray should be requested with a marker on the skin to help to localise it.
Non radio-lucent FBs may be localised by ultrasound. However a normal ultrasound does not completely exclude an FB.
Removing Foreign Bodies
 If an FB is demonstrated, it will usually need to be removed.
If an FB is demonstrated, it will usually need to be removed.
The x-ray is showing glass embedded in the foot.
How should you remove this piece of glass?
Finding an FB may be difficult. If it can be seen or felt, it can be removed under local anaesthesia. If it cannot be seen or felt, the inexperienced doctor should ask advice before trying to remove it. It is not urgent and it may be better to remove it electively.
Undoubtedly the easiest way to remove an FB is under general anaesthesia with the use of a tourniquet and an image intensifier, but this usually requires referral to an orthopaedic surgeon. An experienced doctor may elect to remove a foreign body in the ED under some type of local anaesthesia e.g. a foot block.
If there is more than one FB, the foot should be x-rayed after removal to ensure that there is no remaining FB.
- Fractures of the calcaneum are easily missed on ankle x-rays. Ask for calcaneal views.
- Foot injuries are common in high speed road crashes but may be overlooked if the patient has other, life-threatening, injuries.
- Injuries of the talus and other tarsal bones as well as the tarso-metatarsal joints may be difficult to detect on plain X-rays. If there is a mechanism of injury that suggests the possibility of a serious injury, or if there are clinical signs suggesting a serious injury, then have a low threshold for CT.
- The apophysis at the base of the 5th MT may be misdiagnosed as a fracture.
- Solomon L, Warwick DJ, Nayagam S. Apleys System of Orthopaedics and Fractures 8th Edition. 2001. Arnold. London
- Stiell IG, Greenberg GH, McKnight RD, Nair RC, McDowell I, Worthington JR. A study to develop clinical decision rules for the use of radiography in acute ankle injuries. Ann Emerg Med. 1992;21:384-90.
- May G. In undisplaced, extra-articular calcaneal fracture is the use of a below knee POP associated with longer rehab period. 2006 www.bestbets.org/bets/bet.php?id=1309. accessed 16.3.09
- Martin B, Mackway-Jones K. Support bandaging is best for avulsion fractures of the base of the fifth metatarsal 2001 http://www.bestbets.org/bets/bet.php?id=54 (accessed 16.3.09)
- Dardouri H, Hassan Z. Subungal Haematoma: Trephine drainage versus non-drainage. 2005 http://www.bestbets.org/bets/bet.php?id=972 accessed 18.3.09
- Scott L, Flannery O, Hearns S, Teece, S. Infection risk when trephining Subungal Haematomas with associated closed distal phalangeal fractures. http://www.bestbets.org/bets/bet.php?id=603 accessed 16.3.09]
- Harrison M, Thomas M. 2000. Antibiotics after puncture wounds to the foot. http://www.bestbets.org/bets/bet.php?id=175 accessed 18.6.09

























18 Comments
Thanks for a great discussion of foot injuries
Good overview of foot injuries.
Gave a good overview of the foot injuries, thank you.
great one
Good read.
very informative
Thanks for good article. Useful to repeat this stuff
very useful
very good
very comprehensive synopsis of foot injuries
Very comprehensive overview of foot .
very nice useful information
good info, not exhaustive
Great! Clarified various areas where some degree of of uncertainty lingers in the mind while dealing with foot injuries. Also highlighted areas where mistakes can happen and how to avoid them. Excellent reading for ED physicians.
That was an intense information
Excellent overview of foot injuries, with many clinical nuggets to note. Thanks!
Nicely explained
Very useful and practical information