Author: Clint Gomes, Richard Lowsby / Editor: Jason B Lee / Reviewer: Louise Burrows, Clint Gomes / Codes: SLO4, SLO5, TC2, TP7 / Published: 11/03/2022
Context
Elbow injuries are common and acute elbow trauma accounts for 2-3% of all visits to the emergency department6.
It is important for the emergency physician to have a good knowledge of the elbow joint and to be aware of the common injuries that occur. Injuries are common, both in adults and children, but the fracture patterns in children tend to be different to the adult population due to the nature of the developing bones.
An ability to interpret elbow radiographs is important to detect what may often be subtle injuries. Paediatric radiographs, in particular, can be very difficult to interpret and are complicated further by the gradual appearance of multiple ossification centres during skeletal development.
This session aims to provide an introduction to the common acute traumatic injuries that occur around the elbow joint, and to provide the emergency physician with an understanding of the assessment and initial management of these injuries.
Learning bite
Elbow injuries are common in both adults and children although fracture patterns differ between the two populations.
Anatomy
The elbow is a hinge joint and consists of the humero-ulnar, humero-radial and proximal radio-ulnar articulations. The radial head articulates with the humeral capitellum whilst the trochlear notch of the ulna articulates with the humeral trochlea. Posteriorly the ulna forms the olecranon, which contacts the olecranon fossa of the humerus at full elbow extension.
Anatomy of the joint – The elbow joint allows from 00 to approximately 140-1500 of flexion7.
Learning bite
The elbow is a hinge joint formed by the humerus, radius and ulna.
Hyperextension may be possible and up to 15 is considered normal, especially in women. Movement at the proximal and distal radio-ulnar joints combine to produce 75 of pronation and 80 of supination. When fully extended the elbow joint forms a valgus angle, this is commonly referred to as the carrying angle and is generally greater in women.
Bony landmarks of the elbow palpable on examination are the:
- medial and lateral humeral epicondyles
- olecranon process and proximal ulnar shaft
- head of radius
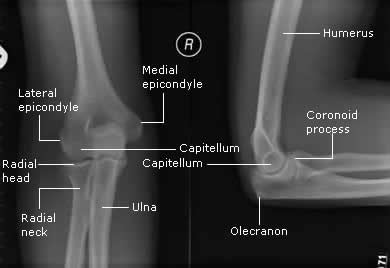
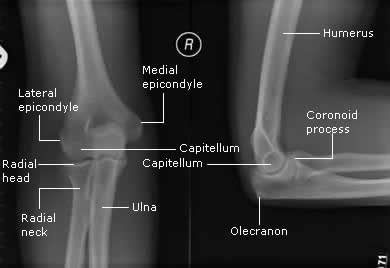
Figure 1: Bony anatomy of the elbow
Ligaments
The lateral and medial collateral ligaments provide joint stability. The nearby annular ligament attaches to the anterior and posterior margins of the radial notch on the ulna and forms a collar around the radial head.
Figure 2: Elbow ligaments
Muscles
Elbow flexion results from the actions of the biceps brachii, brachialis, brachioradialis and pronator teres muscles, which cross the joint anteriorly. The triceps tendon inserts into the olecranon process posteriorly and together with the anconeus muscle is responsible for elbow extension.
Figure 3: Muscles surrounding the elbow joint
Several muscles responsible for wrist and finger flexion have a common insertion into the medial epicondyle (flexor carpi radialis, palmaris longus, flexor carpi ulnaris and flexor digitorum superficialis). Similarly, several extensor muscles insert into the lateral epicondyle (extensor carpi radialis brevis, extensor digitorum, extensor digiti minimi and extensor carpi ulnaris).
Learning bite
Several forearm flexor and extensor muscles insert at the elbow.
Nerves and arteries
The cubital fossa is a triangular depression found anterior to the elbow joint and contains the median nerve, biceps tendon, brachial artery, and radial nerve (deep and superficial branches). The ulnar nerve crosses the elbow joint posteriorly, running behind the medial epicondyle in a groove adjacent to the olecranon. The olecranon bursa is located over the posterior aspect of the olecranon.
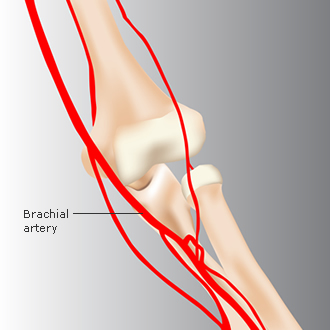
Figure 4: Nerves and artery running across the elbow joint
Initial Assessment

The initial assessment of the patient presenting with an elbow injury should consist of a history, the key points of which include the:
- Mechanism of injury (particularly important in paediatric injuries when non-accidental injury should be considered)
- Onset and location of pain
- Associated symptoms, including sensory disturbance and proximal or distal limb pain
- History of previous elbow injury
Learning-bite
The history of the injury should be taken prior to examination.
Examination
Subsequently the examination route should follow the sequence of:
Look

This should also include the wrist and shoulder. Note any bruising, swelling or deformity.
The medial and lateral epicondyles, along with the olecranon, should form a straight line in full extension and an equilateral triangle in flexion. Disturbance of this alignment should raise the suspicion of a fracture or dislocation.
Learning bite
It is useful to note the alignment of the epicondyles and olecranon in both flexion and extension.
Feel

The bony landmarks mentioned previously should be palpated (medial and lateral epicondyles, olecranon and radial head).
Further palpation, particularly of the radial head, should occur during elbow movement.
Tenderness over the common flexor or extensor tendon insertions in the absence of a history of acute trauma is suggestive of tendinopathy and can be confirmed with special tests.
Learning bite
Careful palpation can help to identify the structure(s) likely to be injured.
Move

Passive and active range of elbow movement should be assessed and should include flexion, extension, supination and pronation. It is important to compare both sides in order to distinguish between normal and abnormal reduced range of movement.
Resisted elbow flexion and extension stresses the biceps and triceps tendons respectively and increased pain on testing may suggest a musculotendinous strain.
Grossly reduced flexion or extension strength, accompanied with pain and localised swelling/bruising, might suggest a rupture of the biceps tendon or avulsion fracture of the triceps insertion.
Learning bite
Movement of both sides should be compared during the examination.
Special Tests
The medial and lateral collateral ligaments should be stressed with valgus and varus forces across the joint in 30 degrees of flexion. Increased pain and/or laxity are suggestive of ligamentous sprain.
Extensor tendinopathy

The common extensor tendon insertion should be palpated during resisted wrist extension with the forearm pronated, increased pain is suggestive of extensor tendinopathy, otherwise known as lateral epicondylosis or ‘tennis elbow’.
Flexor tendinopathy

Similarly, increased pain located at the common flexor tendon insertion during resisted wrist flexion with the forearm supinated, is suggestive of flexor tendinopathy, also known as medial epicondylosis or ‘golfer’s elbow’.
As with all musculoskeletal injuries the neurovascular status of the distal limb should be assessed. Specifically median, radial and ulnar nerve sensory and motor functions should be tested, along with palpation of the radial and ulnar pulses.
Imaging
Figure 5: Normal elbow xray
Important Lines
Anterior Humeral Line
If a line is drawn along the anterior part of the humerus on the lateral radiograph, then it should intersect the middle third of the capitellum. Failure to do this indicates that the capitellum has been displaced. There is often posterior displacement in association with supracondylar fractures.
Figure 6: Normal (left) and abnormal (right) anterior humeral line
The Radio-Capitellar Line
A line drawn through the middle of the radius should always bisect the capitellum since the radial head articulates with the capitellum. This should occur in every direction, no matter which x-ray view is taken. If this is not the case suspect dislocation of the radial head and remember that this can sometimes be associated with ulna fractures (Monteggia fracture-dislocation).
Figure 7: Normal (left) and abnormal (right) radio-capitellar line
Fat Pads
On a normal AP x-ray of the elbow an anterior fat pad is visible due to fat in the joint capsule. It is never normal to see a posterior fat pad because this is hidden in the intercondylar fossa. The diagram below shows a displaced anterior fat pad in association with a posterior fat pad. This is known as the sail sign because of its resemblance to the sails of a boat. In the setting of acute trauma it represents blood in the joint. In the non-trauma setting effusion may be due to an inflammatory cause. Note that if the fracture is extra-articular, then there may not be a joint effusion and therefore the fad pad sign will be absent.
Examine the radial head closely in these injuries as there is often a subtle fracture. Presence of a posterior fat pad has been associated with a 75% rate of occult fracture.
Learning bite
The anterior humeral line, radio-capitellar line and the presence or absence of fat pads can aid x-ray interpretation.
Figure 8: Positive Sail Sign
Ossification Centres
There are six ossification centres in the elbow of a developing child and they occur in a fixed order at sequential times up to the age of 13 years, although these times are variable. It is the presence of these centres that make paediatric elbow x-rays notoriously difficult to interpret. Knowledge of these ossification centres and the age at which they appear will assist the observer in identifying whether a fracture is present or not. A well-known helpful pneumonic for this is CRITOL or CRITOE:
| Capitellum | 1 year |
| Radial head | 3 years |
| Internal (medial) epicondyle | 5 years |
| Trochlear | 7 years |
| Olecranon | 9 years |
| Lateral (External) epicondyle | 11 years |
Note that these ages vary but a broad guide of 1,3,5,7,9 and 11 years is easy to remember.
Figure 9: Ossification centres
Contours
Finally, it is important to analyse all three bones of the elbow joint and follow the contours, looking for irregularities and steps that could indicate subtle disruptions and fractures in the cortex.
Common subtle injuries that may be difficult to identify include undisplaced radial head fractures in adults and undisplaced supracondylar fractures in children. There may often be other clues such as a positive fat pad sign (click on the x-ray to enlarge).
Clearly, the x-ray is an adjunct to your assessment and management should be based on clinical findings and suspicion, rather than x-ray appearances alone.
Whenever a fracture is identified it is essential that the ipsilateral wrist is imaged along with the entire radius and ulna, in order to exclude any associated fractures or dislocations.
Learning bite
It is important to interpret the x-ray in combination with examination findings.
The identification of a bony injury should prompt a search for other associated injuries. This may require additional imaging.
Elbow Dislocation
Elbow dislocation is seen in both children and adults and is usually caused by a fall onto the outstretched hand. In children it is more common than dislocation of the shoulder [2].
Examination may reveal obvious deformity of the elbow. The triangular relationship of the epicondyles and olecranon will be disrupted. It is important to check the distal neurovascular status of the limb due to possible damage to the brachial artery or median and ulnar nerves.
The dislocation is most commonly in a posterior or posterolateral direction and will be confirmed on x-ray, along with the presence of any associated fractures. Associated epicondylar fractures and fractures of the lateral condyle are known to occur in children.
Click on the x-rays to enlarge.
 |
 |
| Fig 1: This lateral view clearly demonstrates posterior dislocation of the elbow. Note the associated fracture fragment. | Fig 2: The AP view of the same injury illustrates some lateral displacement. |
Other Fractures
Radial head fractures
Radial head injuries usually follow a fall onto an outstretched wrist or direct trauma. Radial head fractures usually occur in adults and account for 30% of all adult elbow fractures [3].
The x-ray shows a displaced radial head fracture
Examination may reveal local bruising and swelling. In some cases pain may only be evident with palpation of the radial head during passive forearm pronation. Elbow extension is usually restricted.
Assessment of the wrist should be performed due to the possibility of an Essex-Lopresti fracture-dislocation, consisting of a comminuted radial head fracture with subluxation of the distal end of the ulna.
Radiography may reveal the fracture or merely the presence of a joint effusion.
Learning bite
Pain due to a radial head fracture may only be evident with palpation during passive forearm pronation.
Olecranon fractures
With olecranon fractures the mechanism of injury is usually a fall onto the point of the elbow or onto a semi-flexed outstretched forearm.
The x-ray shows a displaced olecranon fracture
Examination will reveal swelling and tenderness over the posterior aspect of the elbow. Radiography will confirm the diagnosis and also reveal any displacement due to the pull of the triceps tendon.
Identification of paediatric olecranon fractures may be complicated by the appearance of the olecranon ossification centre, which may be bifid.
Learning bite
Care should be taken when attempting to identify or exclude a fracture in a child with an olecranon ossification centre.
Monteggia fracture-dislocation
A Monteggia fracture-dislocation injury comprises of a dislocation of the radial head with an ulna fracture. It may result from a direct blow to the ulna or forced pronation.
The x-ray shows a Monteggia fracture-dislocation with partially visible ulna shaft fracture.
The radiographic appearance of a dislocated radial head (suspect if a line bisecting the radius longitudinally does not pass through the centre of the capitellum) should prompt further imaging of the forearm to exclude an ulna fracture.
Learning bite
Radial head dislocation should raise suspicion of an associated ulna fracture.
Galeazzi fracture-dislocation
A Galeazzi fracture-dislocation injury consists of a radius fracture in combination with dislocation of the inferior radio-ulnar joint at the wrist. The wrist joint should therefore be imaged and closely inspected when a radial fracture is identified.
The x-ray shows a Galeazzi fracture-dislocation
The possibility of combined injuries such as those recognized by Galeazzi and Monteggia illustrates the need to image the elbow, wrist and entire radius and ulna when one bony injury is identified.
Learning bite
The presence of a radius fracture should raise suspicion of associated distal radio-ulna joint dislocation.
Differential Diagnosis (Paediatric)
Supracondylar Fractures
Supracondylar fractures account for 60% of all paediatric elbow fractures and typically follow a fall onto an outstretched hand. The peak incidence occurs between the ages of five and eight years [4].
Children are more prone to supracondylar fractures than adults due to the relatively thin trabeculae of the coronoid and olecranon fossae in this section of the population. Ninety percent of these fractures are caused by hyperextension injury due to ligament laxity. The force is transmitted up through the ulna and into the distal humerus.
Learning bite
Supracondylar fractures are most commonly due to a hyperextension injury.
Signs to look out for on x-ray include presence of fat pads and loss of normal anterior humeral alignment. Undisplaced fractures may only be identified by subtle disruption in the posterior cortex whereas displaced fractures will normally be obvious.
Other Injuries
Lateral condyle fracture
Fractures of the lateral humeral condyle are the second most common elbow fracture seen in children, usually between the ages of four and ten [4].
The x-ray shows a displaced lateral condyle fracture.
It results from a varus force applied through the extended elbow, normally due to a fall onto an outstretched hand. It is commonly displaced by the action of the forearm extensors.
Appearance on x-ray may be subtle so an awareness of the possibility of this injury is necessary when interpreting films.
Learning bite
The radiographic appearance of lateral condyle fractures may be subtle.
Medial epicondyle avulsion injury
Medial epicondyle avulsion injuries tend to occur in adolescents due to valgus stress during a fall on an outstretched hand. There may be associated ulna nerve damage and sometimes dislocation.
The x-ray shows an avulsion of the medial epicondyle.
Radial neck fracture
Radial neck fractures are more common in children due to weak metaphyseal bone and, as with radial head fractures, may be difficult to spot on an x-ray [4].
The x-ray shows a radial neck fracture
Pulled elbow
Pulled elbow is also sometimes known as ‘nursemaid’s elbow’. This injury is seen most commonly in children aged one to five years [4]. There is often a history of traction on the arm of the child although this is not always the case. In some cases the parent may not be willing to volunteer the history or may not have been present when the injury occurred. The child will not be using the arm.
Pulled elbow results from subluxation of the radial head from its normal position encircled by the annular ligament.
Learning bite
A pulled elbow should be suspected following a history of traction to the arm.
Differential Diagnosis (Soft Tissue)

Lateral epicondylosis is also known as ‘tennis elbow’.
This condition often occurs as a result of overuse of the forearm extensor tendons.
Previously known as lateral epicondylitis, the pathological process is thought to be due to failed tendon healing and degeneration rather than acute inflammation.
The patient may complain of a diffuse ache located over the lateral aspect of the elbow. The diagnosis can be made clinically as illustrated previously – the image illustrates assessing for common extensor tendon insertion tenderness.
Learning bite
Lateral epicondylitis is often due to overuse of the forearm extensor tendons.
Medial epicondylosis
Medial epicondylosis is also known as ‘golfer’s elbow’.
This condition is seen less commonly than lateral epicondylosis and is similarly often caused by overuse, this time of the forearm flexor tendons, giving rise to pain over the medial aspect of the elbow.
In 20% of cases there may be associated ulnar nerve symptoms, specifically paraesthesia in an ulnar nerve distribution [5]. The diagnosis should again be made clinically.
Learning bite
Medial epicondylosis is often due to overuse of the forearm flexor tendons.
Olecranon bursitis

Olecranon bursitis is usually the result of direct trauma (such as a fall onto the outstretched elbow) or repetitive friction. It may be acute or chronic and can be associated with crystal arthropathy or inflammatory arthritis. Septic bursitis is most commonly due to Staphylococcus aureus infection and can arise directly from an overlying skin wound.
On examination there is localised swelling, tenderness and possible erythema over the posterior aspect of the elbow. Patients with septic bursitis may be systemically unwell with pyrexia, cellulitis and axillary lymphadenopathy.
Blood tests may reveal an elevated ESR, CRP and white cell count. Septic or crystal-induced bursitis can be confirmed with bursal aspiration and subsequent microscopy and Gram stain.
The procedure for the management of elbow dislocations includes:
Analgesia

Analgesia should be provided prior to attempts to reduce the dislocation. Reduction using short-acting analgesic agents such as Entonox or Penthrox may be possible but in some cases reduction using procedural sedation or even reduction under general anaesthetic may be required.
Fig. 10: Posterior elbow dislocation
Reduction techniques
Several techniques for reduction of a posteriorly dislocated elbow are recognised:
 |
 |
 |
| Fig A: With the elbow flexed to 60 degrees provide traction to the pronated forearm and counter-traction to the distal humerus | Fig B: Lever the olecranon forwards whilst traction is being provided to the forearm | Fig C: Position the patient prone with the abducted humerus resting upon the bed and pronated forearm hanging towards the floor. Provide traction to the forearm and downward pressure to the olecranon |
Post reduction
Reduction should be immediately followed by a further assessment of limb neurovascular status. Successful reduction is then confirmed by repeat x-ray. This will also enable assessment of the new position of any associated fractures.
The reduced elbow can be immobilised in a sling or splint in 90 degrees of flexion. In cases where there are concerns over neurovascular impairment or significant elbow swelling a period of observation should follow. This is due to the possibility of compartment syndrome developing in the forearm fascia or biceps tendon. Outpatient orthopaedic review should subsequently be arranged. Myositis ossificans may later develop as a result of large elbow haemarthroses.
Learning bite
Post-reduction assessment of neurovascular status and repeat x-ray is essential.
Other Fractures
Other fractures can be managed in the following ways:
Radial head fractures
Undisplaced radial head fractures can be managed with a collar and cuff sling and orthopaedic outpatient follow-up.
Further management generally consists of early mobilization to prevent loss of elbow extension. Comminuted or displaced fractures may require manipulation under anaesthetic or internal fixation. Occasionally the radial head may need to be excised and replaced.
Radial neck fractures are seen more commonly in children and are managed similar to radial head fractures. Greater than 20 degrees of angulation in the adult requires reduction.
Figure. 11 Radial head fracture
Olecranon fractures
Undisplaced olecranon fractures can be managed with a back slab in 90 degrees of elbow flexion and orthopaedic clinic follow-up.
Displaced fractures (>2mm) and those with comminution are more likely to require operative fixation and therefore warrant orthopaedic referral.
Learning bite
Undisplaced radial head and olecranon fractures may be managed conservatively.
Figure. 12 Olecranon Fracture
Monteggia fracture-dislocation
Monteggia fracture-dislocation injuries should be referred for reduction and internal fixation.
Paediatric Injuries
Figure 13: Type 2 Supracondylar fracture with posterior fat pad

The procedure for the management of paediatric supracondylar fractures includes:
Analgesia
Initial assessment should include provision of analgesia and a search for associated neurovascular complications.
Intranasal administration of analgesia (diamorphine) is a useful option in children and can delay attempts at intravenous access until topical anaesthesia has taken effect.
Treatment
Undisplaced fractures may be treated with a collar and cuff and can be followed up in fracture clinic. If there is significant pain, a back slab may be a better option.
Displaced fractures should all be referred for manipulation, urgently if circulation is compromised.
Complications
Complications include:
- Cubitus varus (gun stock deformity)
- Malunion and stiffness
- Myositis ossificans
- Nerve injury (most commonly the median nerve)
- Brachial artery (due to stretch and posterior displacement)
- Volkmann’s ischaemic contracture (due to compartment swelling)
Other paediatric injuries can be managed in the following ways:
Lateral epicondyle epiphyseal injury
Undisplaced fractures can be managed in a back slab with orthopaedic follow up.
Displaced fractures often need reduction.
Fig. 14: Lateral epicondyle avulsion
Medial epicondyle avulsion injury
Undisplaced avulsions can be managed conservatively.
Displaced fragments should be referred for reduction.
Radial neck fracture
Treatment is similar to that for radial head fractures:
- Undisplaced fractures can be managed with a collar and cuff sling and orthopaedic outpatient follow-up
- Comminuted or displaced fractures may require manipulation under anaesthetic or internal fixation
Orthopaedic referral is recommended if there is greater than 30o of angulation.
Pulled elbow
The x-ray would appear normal and is therefore not necessary prior to attempted manipulation if clinical suspicion is high.
Traditional reduction is achieved by flexing the elbow to 90o and then fully supinating or pronating the forearm, there may often be an associated click and the child will begin using the arm a short time later.
Learning bite
A pulled elbow can be quickly and easily treated in the emergency department with passive supination/pronation of the forearm.
Soft tissue injuries
Lateral epicondylosis / Tennis elbow
This condition occurs as a result of overuse of the forearm extensor tendons. Previously known as lateral epicondylitis the process is thought to be due to failed tendon healing rather than acute inflammation. The patient may complain of a diffuse ache located over the lateral aspect of the elbow. The diagnosis can be made clinically as described previously.
Management should consist of advice regarding relative rest, ice therapy and analgesia. The condition is often persistent and although corticosteroid injection reduces pain the effects do not appear to last beyond six weeks.
Physiotherapy has an established role, although results at 12 months are comparable with patients who have not received any intervention.
Medial epicondylosis / Golfers elbow
This condition is seen less commonly than lateral epicondylosis and is similarly an overuse injury, this time of the forearm flexor tendons, giving rise to pain over the medial aspect of the elbow. In 20% of cases there may be associated ulnar nerve symptoms, specifically paraesthesia in an ulnar nerve distribution. The diagnosis should again be made clinically. Management should follow that for lateral epicondylosis.
Olecranon bursitis

Treatment is with relative rest, ice therapy and analgesia. A broad arm sling may be required in more severe cases.
Septic bursitis requires antibiotics (intravenous if systemically unwell) as per local policy.
Caution is required when considering aspiration of olecranon bursae since fistula formation is a widely recognised complication of the procedure.
- A subtle fracture may be missed if insufficient attention is paid to the appearance of an elevated anterior fat pad
- Radial head dislocation may not be obvious and should be excluded with use of the radio-capitellar line
- A minimally displaced supracondylar fracture may not be obvious and should be excluded with use of the anterior-humeral line
- Misinterpretation of the paediatric elbow x-ray may result from a lack of knowledge of the appearance of ossification centres
- Associated injuries may be missed if the identification of one bony injury does not prompt a search for others with further radiography
- Neurovascular compromise may be associated with supracondylar fractures and elbow dislocations and should always be assessed
- APPELBOAM A., REUBEN A.D. et al. (2008) Elbow extension test to rule out elbow fracture: multicentre, prospective validation and observational study of diagnostic accuracy in adults and children. British medical journal, doi:10.1136/bmj.a2428.
- STRANGE G, AHRENS W, SCHAFERMEYER R, et al. (2002) Paediatric emergency medicine, 2nd ed. McGraw Hill.
- BISSET L., BELLER E., JULL G. et al. (2006) Mobilisation with movement and exercise, corticosteroid injection, or wait and see for tennis elbow: randomised trial. British medical journal, doi:10.1136/bmj.38961.584653.AE
- BRUKNER P. and KHAN K. (2007) Clinical sports medicine, 3rd ed. Sydney: McGraw-Hill.
- BURRA G. and ANDREWS J.R. (2002) Acute shoulder and elbow dislocations in the athlete. Orthopedic clinics of North America, 33(3), pp. 479-495.
- CICCOTTI M.C., SCHWARTZ M.A. and CICCOTTI M.G. (2004) Diagnosis and treatment of medial epicondylitis of the elbow. Clinics in sports medicine, 23(4), pp. 693-705.
- FARO F. and WOLF J.M. (2007) Lateral epicondylitis: review and current concepts. Journal of hand surgery (American edition), 32(8), pp. 1271-1279.
- HARRIS P., RANSON C. et al. (2008) Atlas of living and surface anatomy. London: Churchill Livingstone.
- JACKSON J.D. and STEIMANN S.P. (2007) Radial head fractures. Hand clinics, 23(2), pp. 185-193.
- KUHN M.A. and ROSS G. (2008). Acute elbow dislocations. Orthopedic clinics of North America, 39(2), pp. 155-161.
- LENNON R.I., RIYAT M.S. et al. (2007) Can a normal range of elbow movement predict a normal elbow x-ray? Emergency medicine journal, 24, pp. 86-88.
- MACAULEY, D. (2007). Oxford handbook of sport and exercise medicine. New York: Oxford University Press Inc.
- McRAE R. (2006). Orthopaedics and fractures, 2nd ed. London: Churchill Livingstone.
- ROSENBLATT Y., ATHWAL G.S. and FABER K.J. (2008). Current recommendations for the treatment of radial head fractures. Orthopedic clinics of North America, 39(2), pp. 173-185.
- SHEPS D.M., HILDEBRAND K.A. and BOORMAN R.S. (2004) Simple dislocations of the elbow: evaluation and treatment. Hand clinics, 20(4), pp. 389-404.
- SKAGGS D. and MIRZAYAN R. (1999). The posterior fat pad sign in association with occult fracture of the elbow in children. Journal of bone and joint surgery (Am), 81, pp. 1429-1433.
- TEJWANI N.C. and MEHTA H. (2007). Fractures of the radial head and neck: current concepts in management. Journal of the American academy of orthopedic surgeons, 15(7), pp. 380-387.
- WYATT J.P., ILLINGWORTH R.N. et al. (2006) Oxford handbook of emergency medicine, 3rd ed. New York: Oxford University Press Inc.


























12 Comments
helpful summary
A good summary, thanks
Informative, thank you.
Helpful summary
Good module
Good article for pitfalls to know
nice case for revision
thnk yu
Great summary, thank you
Very informative thanks
Interesting and important session.
Interesting thank you