Author: Anju Sudhakaran Menon / Editor: Lauren Fraser / Reviewer: Rebecca Ford / Codes: DP2, EnvC8, EnvC9, IP1, SLO1 / Published: 26/05/2023
Lyme disease is a zoonotic disease transmitted by ticks.
In 2020, there were 1262 laboratory confirmed cases of Lyme disease reported in England and Wales by Public Health England, of which only approximately 15% are acquired overseas5. It has been estimated that, in addition to the laboratory-confirmed cases, there are also between 1,000 and 2,000 additional cases of Lyme disease each year in England and Wales that are not laboratory-confirmed5. However, as Lyme disease can’t be diagnosed clinically and does go undiagnosed, the true incidence of Lyme disease is unknown. People of all ages can be affected and both sexes are equally susceptible.
It is most often diagnosed during August to September. This coincides with a tick bite in late Spring, arguably because of increased outdoor activity during this period.
Lyme disease can present with a wide spectrum of clinical signs and symptoms (besides that of the characteristic rash) which can take months or even years to resolve, even with appropriate treatment.
NICE published guidance on the diagnosis and management of Lyme disease in April 2018 (updated in October 2018) on which this Learning Session is based. Their guideline aims to raise awareness of when Lyme disease should be suspected and to ensure that people with suspected Lyme disease are given early and consistent treatment. The guideline committee acknowledged that poor-quality evidence is available on both diagnosis and treatment and has developed a series of research recommendations to improve basic epidemiology, understanding of the natural history of Lyme disease, and to develop diagnostic tests appropriate for UK infections.
Ticks are small, spider-like creatures that feed on the blood of animals, including humans (Figure 1). Once they have fed on an animal infected with one of the four Borrelia species of bacteria that cause Lyme Disease they remain infected for life.
In the UK, the most important tick species to human health is Ixodes ricinus, more commonly known as the sheep, castor bean or deer tick. This species can be found feeding on humans and is the principle vector of Lyme disease. They are commonly found in areas with high humidity and ground vegetation (including urban gardens and parks).
Figure 1: Image of a tick
Figure 2: Lyme Disease: Tick and Host Lifecycle
Humans are at risk of infection throughout the year. Different stages peak at different times of the year (figure 2). The larva and adult stage are high during summer whereas the nymph stage increases during spring and autumn. Most tick bites will not transmit Lyme disease.
Learning Bite
Lyme disease can occur anywhere in the UK, although the south of England and the Scottish Highlands are particularly high-risk areas.
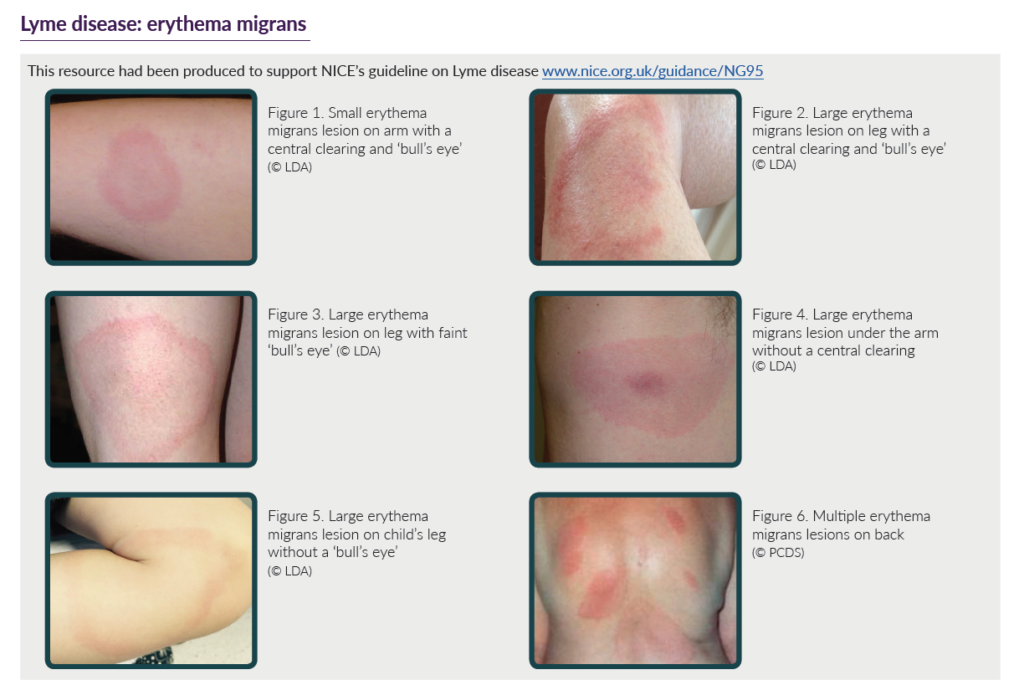
Patients classically present with a red rash that increases in size with central clearing, known as erythema migrans, usually at the site of tick bite. This rash is non-pruritic, and neither hot nor painful.
The rash commonly appears within one to four weeks of the bite (but can present from anywhere between 3 days to 3 months after) and can last several weeks.
Figure 3: Lyme disease: erythema migrans
However, patients can also present with a rash that appears and recedes within the first 48 hours of their outdoor activity. This rash represents a reaction to the tick bite itself. It is more often red, hot, painful and itchy than erythema migrans.
Although this rash is not that of erythema migrans, it would be ideal to check for ticks at this time of presentation. It is worth noting that the original tick bite may have gone unnoticed by the patient.
The possibility of Lyme disease should be considered in patients who present with a combination of the following symptoms because Lyme disease, although uncommon, could be responsible:
- Fevers
- Swollen lymph nodes
- Malaise and/or fatigue
- Nick pain and/or stiffness
- Joint or muscle aches and/or pains that are migratory in nature
- Cognitive impairment such as memory problems and/or difficulty concentrating
- Headache
- Paraesthesia
Learning Bite
In the presence of erythema migrans no investigations are warranted, the rash in itself is diagnostic.
However, in the absence of a rash, serological tests are required to detect the antibodies to the Borrelia bacteria that cause the disease.
A two-tier approach to this serological testing is taken (figure 4): an ELISA test is recommended as the initial investigation given its sensitivity. A more specific confirmatory test is then performed (immunoblot) if the ELISA test is positive or equivocal. Treatment should be initiated whilst awaiting investigation results if there is high clinical suspicion of Lyme disease.
However, there are concerns about the sensitivity of the ELISA test, which can range from 5-100% depending of the timing of the test. It can be falsely negative if done too early or if the patient is immunocompromised. Nevertheless, the specificity of the immunoblot test is high.
The limitations of these tests should be explained to patients so that they are aware of the implications of both false positive and false negative results and how these can occur.
If there is a suspicion of Lyme disease it is best to discuss with your local Infectious Diseases specialist, especially if there is organ involvement. The diagnosis should not be ruled out if there is high clinical suspicion even if the serological tests are negative.
Figure 4: Lyme disease: laboratory investigations and diagnosis
Tests for Lyme disease should only be carried out at laboratories that:
- Are accredited by the UK accreditation service (UKAS) and
- Use validated tests and
- Participate in a formal external quality assurance programme
The drug of choice for Lyme disease is doxycycline; alternatively amoxicillin, azithromycin or ceftriaxone can be used, see figure 5. Please note that azithromycin does not cross the blood brain barrier so ceftriaxone or doxycycline is often preferred, unless contraindicated.
Although there is no difference in cure rate between these antibiotics, a single daily dose of doxycycline is likely to be easier to adhere to for patients than more frequent antibiotic regimens. Treatment is continued for at least 21 days.
All children under 18 with erythema migrans and additional symptoms should be discussed with an Infectious Diseases specialist.
Ask female patients if they might be pregnant before offering antibiotic treatment for Lyme disease as this will affect your antibiotic choice.
If symptoms worsen during treatment, assess for an allergic reaction to the antibiotic. Be aware that a Jarisch-Herxheimer reaction may cause an exacerbation of symptoms but does not usually warrant stopping treatment.
Learning Bite
A Jarisch-Herxheimer reaction is a systemic reaction thought to be caused by the release of cytokines when antibiotics kill large numbers of bacteria. Symptoms include a worsening of fever, muscle pains and headache. The reaction can start between 1 and 12 hours after commencement of antibiotic therapy but can also occur later. It can last for a few hours or 1-2 days. The reaction is self-limiting and usually resolves within 24-48 hours. It was originally reported in the treatment of syphilis but has been documented in tick-borne diseases including Lyme disease, leptospirosis and relapsing fever.
Despite treatment the symptoms of Lyme disease may take months or even years to resolve for a number of reasons:
- The symptoms are caused by alternative diagnosis
- The patient has become re-infected
- There has been a treatment failure
- Symptoms relate to an immune reaction or organ damage
Given the risk of treatment failure, a second (different) antibiotic course should be considered in patients with on-going symptoms despite an initial course of antibiotics.
Consider discussion with a national reference laboratory or referral to a specialist appropriate to the patients symptoms, if they are ongoing after two courses of antibiotics for Lyme disease. Do not routinely offer further antibiotics.
It should be explained to patients with ongoing symptoms following appropriate treatment for Lyme disease that:
- Continuing symptoms may not mean they still have an active infection
- Even after treatment, symptoms may take months or even years to resolve
- Permanent damage from the infection may result in some symptoms
- It is not possible to diagnose active infection using the existing testing methods – an alternative diagnosis may explain their symptoms
Consider the need to support patients with on-going symptoms after treatment for Lyme disease by referral to other services e.g referral to adult social care for a care and support needs assessment or communication with a child or young persons school or higher education regarding graded return to activity as appropriate.
Figure 5: Lyme disease: Antibiotic choices – see here for the BMJ infographic
| Age | Disease | Antibiotic of choice |
| 9 years and above | Erythema migrans
Single nerve involvement
Organ involvement (in HD unstable carditis and CNS involvement IV ceftriaxone is drug of choice) |
doxycycline , amoxicillin, azithromycin (PO)
Doxycycline, amoxicillin(PO)
IV ceftriaxone, doxycycline, amoxicillin(PO) can be tried |
| <9 years | Erythema migrans
Single nerve involvement
Organ involvement |
Amoxicillin and azithromycin PO
Amoxicillin
IV ceftriaxone |
There is no vaccine for Lyme disease. In 1998 LYMErix, the FDA approved vaccine against Lyme disease, was introduced to the market. It was proven to be 80% effective in prevention of the disease. Nonetheless, it was withdrawn within a matter of 3 years because of poor public demand and concerns regarding safety which were never scientifically proven.
Therefore, raising tick awareness is the only pragmatic way to reduce the incidence of Lyme disease. It is necessary to engage in public awareness programs such as campaigns and signposting.
Essentially Lyme disease can be prevented at three stages:
- Before the tick bite
- During the event of tick bite
- After the tick bite
The definitive way to prevent Lyme disease is to promote tick awareness, early tick bite identification and appropriate tick removal.
- Marques AR et al. Lyme Disease: A Review. January 2010, Volume 10, Issue 1, pp 1320.
- National Institute for Health and Care Excellence. Lyme disease NICE guideline [ng95] . Published: 11 April 2018.
- Cruickshank M, OFlynn N, Faust S. Lyme disease: summary of NICE guidance. BMJ. Published 12 April 2018.
- Janak Koirala et al. Lyme disease – Approach | BMJ Best Practice. Last reviewed June 2019.
- Public Health England. Lyme disease epidemiology and surveillance. Updated 14 April 2022. [Accessed May 9, 2023].
- Centers for Disease Control and Prevention. Lyme disease vaccine.
- Lyme disease, Pg 130 Kumar and clark Clinical medicine, eight edition 2012.







16 Comments
Informative
One of the best resources I’ve seen so far, well done
well presented, BMJ infographic topps
Concise and easy to understand
liked it
Well presented
Very well presented with good illustrations.
good overview
good review
Got to know facts of Tick bite unknown to me
Very clear review of borrelia burgdoferi infection and its treatment.
Good review travel history and history of recent outdoor activity becomes important
GOOD article to recapitulate
Informative
nice overveiw
Very well presented description of the topic and good learning