Author: Khalek Adham / Editor: Jason M Kendall / Reviewer: William Gibbs / Codes: AC1, AP1, AP2, AP3, AP4, DC11, PhP1, RP1, RP2, SLO1, SLO3 / Published: 04/06/2011 / Reviewed: 23/11/2023
The sudden nature and type of symptoms experienced in hypersensitivity reactions mean they are a common reason for attending the Emergency Department. Angioedema and Urticaria (hives) can have an allergic or non-allergic aetiology. They can be present in isolation or as part of a wider systemic response, such as in anaphylaxis. Basic knowledge of the pathophysiology of these conditions will help you recognise the type of reaction and treat patients effectively from the outset.
Pathophysiology
Urticaria (hives) is histamine mediated localised oedema of the dermis. Mast cell degranulation and histamine release produces vascular dilation and transudation of fluid from the affected vessels in the skin. Urticaria can be present in isolation as part of a mild IgE mediated reaction to an allergen or in reaction to another stimulus such as cold or heat or occur as part of a syndrome such as anaphylaxis.
Angioedema (AE) is pathogenetically similar to urticaria but involves the deeper dermal and subcutaneous tissue. The aetiology of angioedema can be either allergic (IgE and histamine mediated as in urticaria) or non-allergic. 90% of attacks of angioedema are of the allergic type. Non-allergic AE can be further subdivided (1) into drug induced (e.g. ACE-inhibitors), Hereditary (C1-esterase-inhibitor deficiency), Acquired, Idiopathic and Pseudoallergenic (see Diagram). Non-allergic angioedema is generally mediated by bradykinin.
Drug reactions can cause angioedema through several of the above mechanisms. Those eliciting a Type 1 hypersensitivity reaction will produce angioedema within minutes whereas those causing angioedema by inhibiting bradykinin may not be seen for months (2). The commonest drug classes associated with angioedema are listed in the table below.
| Top 10 drugs / drug classes associated with angioedema (2) |
| ACE inhibitors |
| Bupropion |
| Vaccines |
| Selective Serotonin Reuptake Inhibitors (SSRIs) |
| COX-II Inhibitors |
| Angiotensin 2 antagonists |
| Other antidepressants |
| Non-steroidal anti-inflammatory drugs (NSAIDS) |
| Statins |
| Proton Pump Inhibitors |
HAE is an autosomal dominant condition caused by C1 esterase inhibitor deficiency or functional deficiency. This can be confirmed clinically by low levels of C4 and C1 esterase inhibitor function. The exact prevalence of hereditary angioedema (HAE) is unknown with approximately 1 in 10,000 to 1 in 50,000 people affected (3).
Signs & Symptoms
Urticaria produces wheals and papules of non-pitting, oedematous, erythematous and intensely pruritic skin (see Figure 1). These can appear as crops mainly on the limbs and trunk and can spontaneously resolve quickly.
Figure 1. Urticaria (Hives) (4)

Angioedema involves the deeper dermal structures with little pruritis. It commonly involves swelling of the face, lips (see Figure 2), mouth, tongue, extremities (see Figure 3) and the genitalia in men. Laryngeal involvement can produce stridor and lead to complete airway obstruction. Angioedema is also associated with abdominal symptoms caused by bowel wall oedema, such as colic-like pain, nausea, vomiting and diarrhoea. However cutaneous attacks are the most common form.
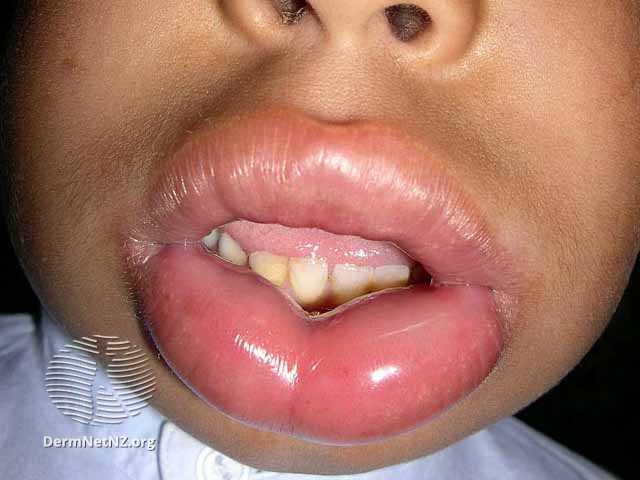
Figure 2 Angioedema of the lips (5)
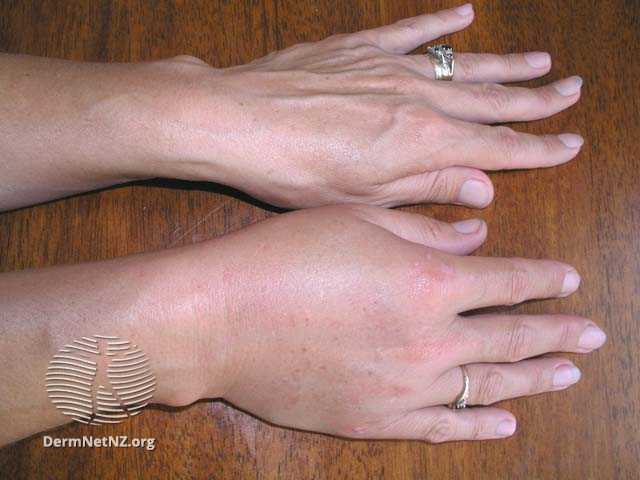
Figure 3 Angioedema of the hand (6)
Symptoms can occur singly or in combination; acute urticaria presents with angioedema in about 50% of cases and alone in 40% of cases (5). Angioedema presents alone in approximately 10% of cases which should prompt consideration of a non-allergic form.
| Allergic Angioedema | Non-Allergic Angioedema | Anaphylaxis |
| Anatomically localised attack | Anatomically localised attack | Systemic symptoms |
| Urticaria | Gradual onset | Rapid onset and progression |
| Pruritis | No Pruritis | Respiratory failure (wheeze, fatigue, cyanosis, hypoxia, tachypnoea) |
| Normotension | Previous identical episodes | Cardiovascular Collapse (Diaphoretic, hypotensive, tachycardia, drowsiness) |
| Abdominal pain | ||
| Normotension |
Measurement of mast cell tryptase can be helpful to confirm anaphylaxis if the diagnosis is uncertain (6). Levels generally peak at 1-2 hours after the onset of symptoms, so a sample should be taken within 2 hours of onset if possible, and no later than 4 hours. Further samples can be taken later during the episode, and/or at follow up in clinic Serial samples have higher specificity/sensitivity for diagnosis. A normal mast cell tryptase does not exclude anaphylaxis.
Where angioedema is suspected to be non-allergic in origin, consider testing C4 levels – C4 may be low where angioedema results from C1 inhibitor deficiency (11).
- Evolving Anaphylaxis
- Cellulitis
- Erisipelas
- Lymphoedema
- SLE
- Contact Dermatitis
Assessment of potentially life-threatening conditions should follow a structured ABC pattern. The initial management goals in acute urticaria and angioedema are airway protection and cardiovascular stability.
If an evolving anaphylactic reaction is suspected then treatment should follow the Resuscitation Council algorithm (6).
Bradykinin-mediated angioedema often does not respond to treatment with epinephrine, anti-histamines or corticosteroids, and alternate treatment strategies are required.
Mild Urticaria and Allergic Angioedema
Urticaria as a sole symptom is unlikely to be life-threatening. In the absence of airway compromise, treatment with H1-receptor blockers (e.g. chlorpheniramine) is indicated. As 85% of histamine receptors in the skin are of the H1 type with the remainder being H2, there is a theoretical benefit to treatment with H2-receptor blockade (e.g. cimetidine, ranitidine) in a histamine mediated reaction, and one randomised controlled trial has shown faster initial symptom resolution using a combination of both H1 and H2 antagonists (7).
Anti-histamines (as above) are also the first-line treatment for mild allergic angioedema.
Severe Allergic Angioedema and Anaphylaxis
In severe attacks of allergic angioedema and anaphylaxis, intramuscular epinephrine is first line treatment. Its adrenergic actions address both peripheral vasodilatation and oedema formation (mediated via alpha adrenoceptors) and inhibit further mediator release (mediated via beta adrenoceptors). Emergency airway protection by a cuffed endo-tracheal tube may be required if laryngeal or oropharyngeal swelling threatens airway occlusion.
Where hypotension or shock is present, IV fluids should be given early (6).
The patient should be treated in a supine or sumi-recumbent position, and sudden changes in posture should be avoided (6), as these may result in cardiovascular collapse.
Resuscitation Council UK guidelines no longer recommend routine use of corticosteroids in the treatment of anaphylaxis. Antihistamines are considered a third line treatment for anaphylaxis (6).
Hereditary Angioedema
Patients with known HAE may have a printed treatment plan.
A number of agents may be used for prophylaxis of HAE attacks (8), including:
- Tranexamic acid (TXA), which works by inhibiting conversion of plasminogen to plasmin, a key step in the autoamplification cycle that generates bradykinin;
- C1 estersase inhibitor concentrate (Cinryze);
- Anabolic steroids such as stanozolol, which have an uncertain mechanism of action;
- Plasma kallikrein inhibitors (Berotralstat or Lanadelumab) which prevent formation of bradykinin.
Attacks of HAE can be treated with Icatibant (a bradykinin B2 receptor antagonist). Patients may have administered a dose of Icatibant at home prior to attending ED. Icatibant is administered as a single subcutaneous injection and has been shown to start producing symptomatic improvement in under an hour (9).
C1 esterase inhibitor concentrate (Berinert or Cinryze) can be given once the patient arrives in ED. If these agents are not available, C1 esterase inhibitor is also found in fresh frozen plasma (FFP) and two units are effective in treating an attack (5).
TXA can also be used for acute management.
Drug Induced Angioedema
If angioedema is suspected to have been caused by a medication such as an ACEi or NSAID, this medication should be immediately discontinued and avoided in future.
For airway or life-threatening drug induced angioedema, seek early specialist advice. Treatments such as Icatibant, Berinert, TXA or FFP may be considered.
Patients who have experienced urticaria alone do not need formal follow up and can be discharged from the emergency department. They should be advised to avoid the precipitating cause (if known) and to take oral anti-histamines for further attacks. Similar advice can be given to those presenting with mild to moderate angioedema who have only required treatment with anti-histamines.
Drug precipitants for the attack should be sought and discontinued if implicated. Patients experiencing ACE inhibitor related angioedema will need their ACE inhibitor discontinuing and replacing with another anti-hypertensive agent. Whilst angiotensin II receptor antagonists (ARBs) have also been associated with angioedema in susceptible individuals (10), the risk of cross reactivity is believed to be low, and ARBs can potentially be trialled in those who have previously experienced ACEi induced angioedema (11).
Those patients who have had a severe attack requiring epinephrine or those who are suspected of having a diagnosis of HAE will need follow-up in an allergy clinic for formal diagnosis. Comparison of mast cell tryptase levels taken during an attack with those during convalescence can aid diagnosis of an allergic attack. These patients should also be considered for an epipen prescription.
- Urticaria and Angioedema can be presenting signs of both allergic and non-allergic disease
- Antihistamines +/- Epinephrine are the first line treatment in both conditions. (Level of evidence 4)
- Addition of an H2 receptor blocker may speed initial symptoms resolution. (Level of evidence 2)
- Angioedema due to hereditary C1 esterase inhibitor deficiency will not respond to normal management and should be treated with a bradykinin receptor antagonist (Icatibant), C1 esterase inhibitor concentrate or fresh frozen plasma. (Level of evidence 3)
Safety Pearls and Pitfalls
The correct identification of the likely type of angioedema the patient is experiencing is critical for allowing correct treatment to be started. Rapid onset with urticaria should suggest an allergic pattern while recent (within months) commencement of a new medication should prompt thought of a drug induced angioedema. Previously undiagnosed HAE sufferers may describe several prior occurrences of non-pruritic attacks without explanation or have attacks that do not respond to anti-histamine therapy.
- Bas M, Adams V, Suvorava T, Niehues T, Hoffmann TK, Kojda G. Nonallergic angioedema: role of bradykinin. 2007 Aug;62(8):842-56.
- West Midlands Centre for Adverse Drug Reaction Reporting. Drug Induced Angioedema. [Online] [Cited: 22 May 2010.]
- Agostini A, et al. Hereditary and acquired angioedema: problems and progress: proceedings of the third C1 esterase inhibitor deficiency workshop and beyond. J Allergy Clin Immunol. 2004 Sep;114(3 Suppl):S51-131. doi: 10.1016/j.jaci.2004.06.047.
- Angioedema. Drugs.com [Online] [Accessed: Nov 2023]
- Marx, John A, [ed.]. Rosens Emergency Medicine. s.l. : Mosby Elselvier, 2006. p. 1835. Vol. 2.
- Emergency Treatment of Anaphylaxis, Guidelines for Healthcare Professionals. Resuscitation Council UK, May 2021.
- Lin RY, Curry A, Pesola GR, et al. Improved outcomes in patients with acute allergic syndromes who are treated with combined H1 and H2 antagonists. Ann Emerg Med. 2000 Nov;36(5):462-8.
- Gompels MM, Lock RJ, Abinun M, Bethune CA, et al. C1 inhibitor deficiency: consensus document. Clin Exp Immunol. 2005 Mar;139(3):379-94. doi: 10.1111/j.1365-2249.2005.02726.x.
- Bork K, Frank J, Grundt B, et al. Treatment of acute edema attacks in hereditary angioedema with a bradykinin receptor-2 antagonist (Icatibant). J Allergy Clin Immunol. 2007 Jun;119(6):1497-503.
- Fuchs SA, et al. Are Angiotensin II Receptor Antagonists Safe in Patients With Previous Angiotensin-Converting Enzyme Inhibitor-Induced Angioedema? Hypertension 37 1; 2001: E1 .
- Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018 Jun;71(6):1269-1324. doi: 10.1161/HYP.0000000000000066. Epub 2017 Nov 13. Erratum in: Hypertension. 2018 Jun;71(6):e136-e139. Erratum in: Hypertension. 2018 Sep;72(3):e33. PMID: 29133354.





24 Comments
nicely explained
Nice presentation and good way of presentation to from Anaphylaxis.
very nice presentation and information enough for saq preparation
Good one!
good one
Well done!
Good article to read
crisp and cosice
excellent
nice but old information
good description of urticaria and angioedema,how ro suspect hereditory angioedema and when to consider epipen .
nice reviews it still recommended the addition of H2 blocker?
Concise and informative. The link to the UK resuscitation council for 2021 guidelines is very helpful.
short and sweat
Great!
very good and informative
Useful and informative article
Great
THANKS
short brief explanation and differentials and management with good learning with respect to patients presenting to ED
Nicely explained.
very useful and helpful
very good and informative
Nice fruitful topic